Postmenopausal endometriosis is a condition many misunderstand. While it’s often assumed endometriosis resolves after menopause, the disease can persist or even appear for the first time. In postmenopausal women, it often takes a more fibrous, less bleeding form that’s harder to spot clinically. This article explains why pelvic MRI is key to diagnosing postmenopausal endometriosis, how MRI findings guide decisions about malignancy risk and surgical plans, and how imaging works hand-in-hand with medical treatments and hormone therapy choices. You’ll learn to recognize what fibrous nodules look like on imaging, understand MRI protocol priorities for older patients, and follow a clear path from diagnosis to treatment that highlights the power of multidisciplinary care.
This content addresses key clinical questions: defining postmenopausal disease, MRI advantages versus ultrasound, MRI signs of cancerous changes, treatment options including excision surgery and medical therapies, and how you can access specialized, personalized care. The Endometriosis Center of Excellence, led by board-certified specialist Dr. Rachael Haverland (trained at the Mayo Clinic), uses advanced imaging and a multidisciplinary pathway to translate MRI findings into individualized treatment plans for postmenopausal patients, which we’ll touch on briefly before exploring the clinical details.
What Is Postmenopausal Endometriosis and How Does It Differ from Premenopausal Disease?
Postmenopausal endometriosis refers to endometriosis lesions that continue after natural or surgical menopause, or even appear for the first time in a low-estrogen environment. These lesions often transform from bleeding cysts into more fibrous, solid nodules with increased adhesions. The mechanism involves ongoing inflammation, local estrogen production through aromatase activity in ectopic tissue, and progressive fibrosis. This lessens the classic signs of cyclical bleeding, making it harder to detect clinically. For you and your clinicians, the practical value is that symptoms can be more subtle, making imaging vital for mapping the disease because physical exams and CA-125 tests are less precise for older patients. Understanding these differences helps us know when to prioritize MRI, especially if deep infiltrating disease, pelvic pain, or suspicious masses are a concern after menopause.
What Defines Postmenopausal Endometriosis?
Postmenopausal endometriosis is defined by the presence of endometriosis in women who have stopped having menstrual cycles, whether from natural menopause, oophorectomy, or long-term amenorrhea. Lesions can be lingering remnants from earlier disease or develop due to local estrogen production. The way the disease works changes, leaning towards collagen buildup and fibrous tissue, showing up as low T2 signals on MRI and with fewer signs of bleeding compared to premenopausal endometriomas. Clinically, diagnosis depends more on imaging and tissue analysis since menstrual symptoms are gone, and the fibrous nature often leads to persistent pelvic pain or symptoms tied to specific organs. Knowing if it’s persistent or new helps guide how we monitor and manage it.
What Are the Common Symptoms and Diagnostic Challenges After Menopause?
Symptoms commonly include persistent pelvic pain, newly painful intercourse, bowel or bladder dysfunction, and an ovarian or uterine mass found by chance. These presentations can look like other conditions such as pelvic organ prolapse, pelvic inflammatory disease, or even cancer, making diagnosis tricky. Because cyclical pain is typically absent, clinicians may mistake symptoms for other age-related pelvic issues, delaying further investigation or specialist evaluation. Imaging—especially pelvic MRI—becomes critical to tell the difference between fibrous nodules, adhesions, and solid growths from other conditions, and to help decide if a biopsy or excision is needed. Getting imaging done early when symptoms continue offers clearer diagnostic paths and speeds up getting you the right care.
Which Risk Factors Influence Postmenopausal Endometriosis?
Several factors increase the chance of persistent or noticeable disease after menopause: a prior history of endometriosis, the use of hormone replacement therapy (particularly estrogen used alone), obesity (through estrogen produced in other body tissues), and selective estrogen-modulating therapies like tamoxifen. Each of these increases local or systemic estrogen exposure or inflammation, which can keep ectopic endometrial tissue active or reactivate it and, in some settings, increase the need to watch for cancerous changes. Clinicians should include risk assessment in monitoring plans, balancing symptom relief with the risk of malignancy when recommending imaging or therapy.
Why Is MRI the Preferred Imaging Modality for Postmenopausal Endometriosis Diagnosis?
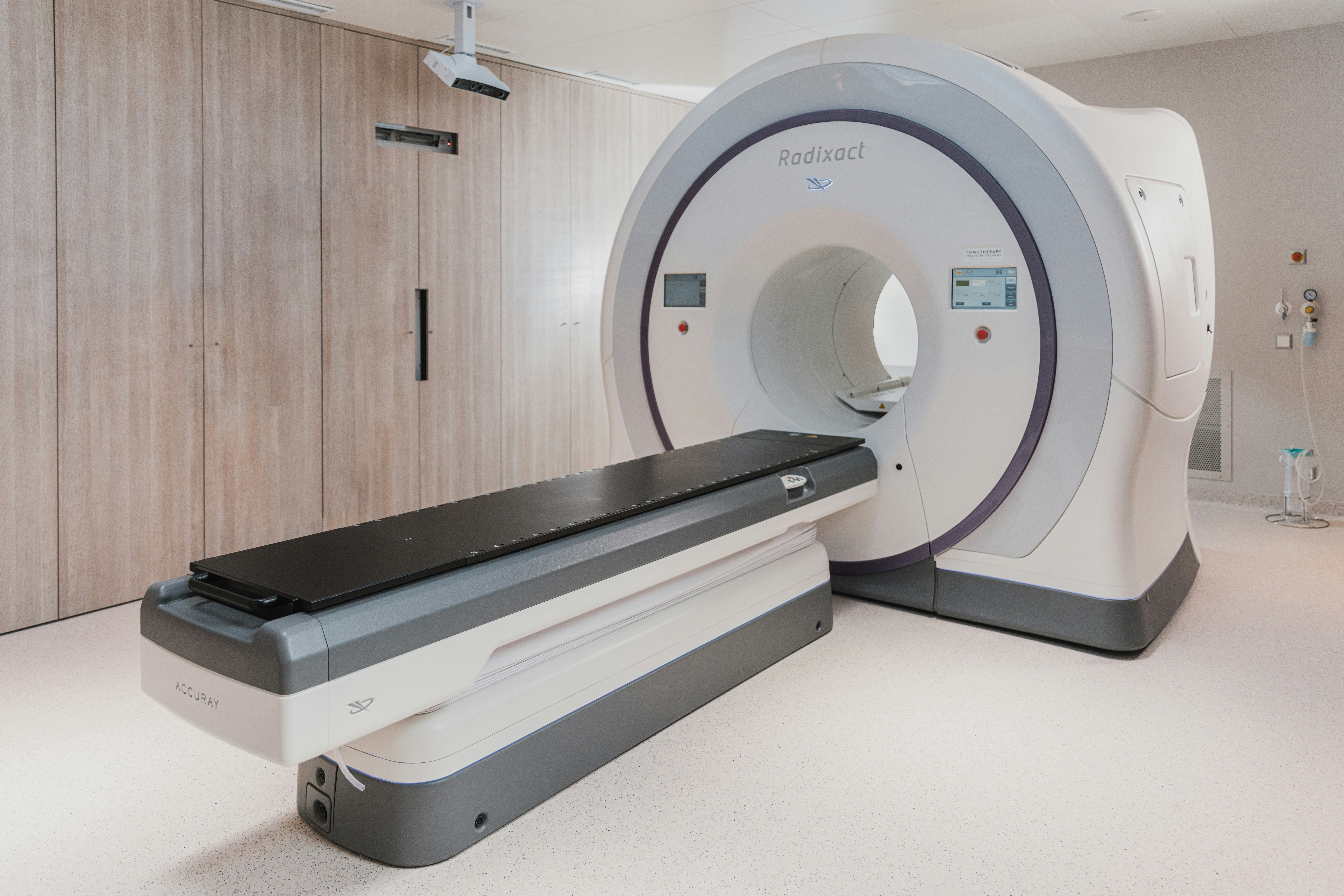
Pelvic MRI offers excellent soft-tissue detail, a wide view to map disease in multiple areas, and the ability to clearly show solid fibrous nodules versus bleeding cysts. These advantages make MRI the go-to choice for postmenopausal patients, where fibrous and solid growths are more common. MRI helps surgeons plan by clearly showing how lesions relate to pelvic organs, pinpointing deep infiltrating endometriosis and adhesions, and spotting solid areas that light up with contrast, which could signal cancerous changes. Current research and radiology practice emphasize specialized pelvic protocols and interpretation by radiologists who truly understand endometriosis to get the most accurate diagnosis.
What Makes MRI Superior to Ultrasound for Postmenopausal Endometriosis Imaging?
MRI is better than ultrasound for deep infiltrating disease and for seeing adhesions and how fibrous nodules are spread out. This is because MRI can view the pelvis from multiple angles and offers superior tissue contrast, making it less dependent on the person performing the scan. Ultrasound still has its benefits—it’s more affordable, readily available, and great for simple ovarian cysts—but it struggles with small, hard-to-reach, or mostly fibrous lesions. MRI is our recommended next step when deep or complex disease is highly suspected, when ultrasound results aren’t clear, or when detailed mapping is needed before excision surgery.
Before we look at the comparison table, here are some key points it will summarize, helping clarify why we choose certain imaging in practice.
What Are the Specific MRI Features of Postmenopausal Endometriosis?
Postmenopausal lesions often show up as low T2 signal fibrous nodules, irregular solid masses, or adhesions that change the normal pelvic structure. The classic T1 bright bleeding cysts (with T2 shading) are less frequently seen. Additional MRI features include dark spots on T2, blurring of the fat layers between organs, solid growths within cysts that light up with contrast, and restricted diffusion in areas with many cells or where cancer might be developing. Our radiologists carefully report lesion size, how they enhance with contrast, and their relationship to the bowel, bladder, and ureters. This vital information guides surgical planning and helps us assess malignancy risk.
The radiologist’s expertise is vital in spotting subtle yet important findings on MRI, particularly in postmenopausal women where endometriosis can often be overlooked.
How Do Advanced MRI Protocols and Expert Interpretation Improve Diagnosis?
A specialized pelvic MRI protocol for endometriosis usually involves high-resolution T2-weighted images from various angles, T1-weighted images with and without fat suppression, contrast-enhanced imaging if cancer is suspected, and diffusion-weighted imaging to check cell density. Adjusting slice thickness, field-of-view, and using medications to reduce bowel movement can improve how well we see small nodules and adhesions. When radiologists experienced in deep infiltrating endometriosis interpret the scans, it leads to better lesion detection, fewer missed diagnoses, and reports that directly guide decisions on how much to excise and whether a multidisciplinary surgical team is needed.
Fine-tuning MRI protocols is crucial for an accurate diagnosis, especially for deep pelvic endometriosis. Research continues to explore various preparation techniques and sequences to improve detection.
How Does MRI Help Differentiate Benign Endometriosis from Malignant Transformation
MRI helps us tell the difference between benign endometriosis and cancerous changes by spotting imaging features that suggest increased cell activity, new blood vessel growth, and complex structures. These findings help us determine the urgency for biopsy, surgical excision, and cancer staging if necessary. In postmenopausal patients, a growing endometrioma, a new solid growth within a cyst that lights up with contrast, or restricted diffusion should raise a red flag and lead to quick evaluation. MRI therefore acts as both a diagnostic tool and a way to monitor the condition, allowing for comparisons over time and multidisciplinary discussions between gynecology, radiology, and oncology when suspicious features arise.
What Is the Risk of Malignant Transformation in Postmenopausal Endometriosis?
The estimated risk of endometriosis turning cancerous varies depending on the lesion type and study, but it’s generally cited in medical literature as around 1–3% for endometriomas. Factors that increase this risk include age, long-term estrogen exposure, and lesions that are large or growing quickly. Being postmenopausal means we’re extra vigilant because lesions are typically expected to be quiet. Therefore, any new growth or change in symptoms after menopause calls for prompt imaging and a discussion about surgical management. Recognizing these risk estimates helps us customize follow-up schedules and when to consider a biopsy or excision.
Which MRI Features Indicate Possible Malignancy?
Certain MRI findings increase concern for malignancy: a solid growth within a cyst that lights up with contrast, the disappearance of the typical T2 shading in a previously bleeding endometrioma, significant restricted diffusion (bright signal on DWI with low ADC), and a quick increase in lesion size on follow-up scans. When these features are present, we recommend steps like checking tumor markers, getting follow-up imaging sooner, a targeted biopsy if possible, and multidisciplinary surgical planning. Spotting these imaging signs early helps us get to a definitive diagnosis faster.
Before the table, it’s helpful to remember that connecting MRI features to their clinical meaning helps doctors turn radiology findings into clear treatment steps.
Why Is Ongoing MRI Surveillance Important for Postmenopausal Patients?
Ongoing MRI surveillance is important when initial scans show unclear ovarian masses, solid growths that light up with contrast, or if you have high-risk factors like using estrogen alone. Repeated MRI scans allow us to objectively track growth over time and any changes in the lesions. Our recommended approach is personalized: a repeat MRI in a shorter timeframe (e.g., 3 months) for suspicious changes, or annual imaging for stable, low-risk lesions. We’d escalate care if there’s an increase in size, new enhancement, or worsening symptoms. Combining MRI results with your clinical exam and tumor markers helps us pinpoint the best time for a biopsy or definitive surgical treatment.
What Are the Comprehensive Treatment Options for Postmenopausal Endometriosis?
Managing symptomatic or suspicious postmenopausal endometriosis carefully balances surgical excision, medical therapy, and thoughtful hormone management, all customized to your goals, other health conditions, and malignancy risk. Excision surgery is still the gold standard for symptomatic disease and for removing lesions that raise concerns for cancer. Pre-surgery MRI mapping greatly improves how completely we can remove the disease and reduces the chance of missing anything. Medical treatments—mainly aromatase inhibitors and progestogens—can help reduce lesion activity or symptoms when surgery isn’t an option or as an additional therapy, but they are less effective for dense, fibrous lesions that are more structural than hormonally active. Hormone replacement therapy needs a personalized assessment, focusing on combined or cautious approaches if you have a history of endometriosis.
How Does Excision Surgery Provide Effective Relief for Postmenopausal Women?
Excision surgery focuses on completely removing endometriosis implants and related adhesions. For postmenopausal patients, this can directly ease organ-specific pain and lower the risk of missing cancerous changes. Successful outcomes rely on detailed pre-surgery mapping and the surgeon’s expertise. Minimally invasive techniques—like laparoscopic or robotic-assisted excision—are preferred when possible to reduce complications. MRI findings help guide how much tissue needs to be removed and if a multidisciplinary surgical team (like colorectal or urologic surgeons) is needed during the procedure. Recovery is typically quicker with minimally invasive techniques, and precise surgical planning, guided by MRI, helps reduce the need for repeat surgeries.
What Medical Management Options Support Postmenopausal Endometriosis Care?
Medical options for postmenopausal endometriosis aim to suppress local estrogen production or adjust the hormonal environment. Aromatase inhibitors (which stop local estrogen production) and progestogens can be used to manage symptoms or lessen lesion activity when immediate surgery isn’t an option. These medications have potential side effects that need monitoring—aromatase inhibitors for bone density and progestogens for metabolic or mood changes—and are less effective for dense, fibrous nodules that are more about structure than hormone activity. Thus, medical therapy often acts as supportive care or a temporary solution until definitive excision can be performed.
Before we look at the treatment table, remember that combining surgical and medical options requires a personalized risk-benefit analysis, especially for postmenopausal patients.
How Should Hormone Replacement Therapy Be Navigated with Endometriosis History?
Approaching HRT for patients with a history of endometriosis calls for a personalized risk assessment. Estrogen used alone could potentially stimulate any remaining endometriosis tissue and might increase the risk of recurrence or even cancer, whereas combined estrogen-progestogen therapies offer protective benefits for endometrial tissue. Decisions should involve a collaborative discussion between your gynecologist, endocrinologist, and you, considering the severity of your menopausal symptoms, imaging findings, and prior disease history. Alternatives to systemic estrogen—like topical or non-hormonal approaches—might be suitable for some patients to reduce the chance of disease reactivation while still addressing quality-of-life concerns.
How Can Patients Benefit from Personalized Care at Endo Excellence Center?
The Endometriosis Center of Excellence offers a patient-centered, multidisciplinary approach that brings together advanced imaging, evidence-based medical care, and gold-standard excision surgery when needed. This is all guided by our board-certified leadership and a deep commitment to your individual outcomes. Led by Dr. Rachael Haverland, trained at the Mayo Clinic, the center focuses on precise pre-surgery MRI mapping, minimally invasive excision techniques, and coordinated support for your bowel, bladder, and emotional well-being. For patients navigating diagnosis after menopause, this integrated approach ensures that your MRI findings lead to clear, personalized management plans that carefully balance symptom relief, cancer monitoring, and menopausal care.
What Makes Endo Excellence Center’s Approach Unique for Postmenopausal Endometriosis?
The Endometriosis Center of Excellence’s model brings together a specialist-led clinical pathway with multidisciplinary coordination to meet the complex needs of postmenopausal patients. We use MRI to guide both surgical planning and long-term monitoring. Dr. Rachael Haverland’s board certification and Mayo Clinic training ensure an authoritative clinical approach, focused on genuine care rather than marketing hype. The practice prioritizes gold-standard excision surgery when appropriate, along with minimally invasive options to shorten your recovery time. Support services—including bowel and bladder assessment and emotional care—are woven into your treatment plan to address the full impact of endometriosis, not just what we see on scans.
How Can Patients Schedule a Consultation for MRI and Treatment?
Your journey begins with an initial consultation where we review your past records and imaging, then agree on a targeted diagnostic path. This often means prioritizing a specialized pelvic MRI if we suspect deep or complex disease. Please bring any previous ultrasound or MRI reports, a clear history of your symptoms, and any surgical records to your appointment to help us streamline your plan. Our contact phone and address are provided for easy scheduling and directions. Our diagnostic pathway typically involves a specialized pelvic MRI with specific sequences, a thorough review by an experienced radiologist, and a multidisciplinary discussion to decide if medical therapy, ongoing monitoring, or excision surgery is the best next step for you.
Is MRI Effective for Detecting Postmenopausal Endometriosis?
Yes, pelvic MRI is exceptionally effective for detecting deep infiltrating and fibrous endometriosis in postmenopausal patients. It offers superior soft-tissue contrast and multiplanar mapping compared to ultrasound. We prefer MRI when ultrasound results are unclear, when lesions are suspected to involve the bowel or bladder, or when detailed pre-surgery mapping is essential. Interpretation by radiologists with expertise in endometriosis further enhances diagnostic accuracy and provides actionable reports.
The effectiveness of MRI in detecting postmenopausal endometriosis is well-established, offering clear advantages over other imaging methods for complex cases.
Can Hormone Replacement Therapy Reactivate Endometriosis?
HRT—especially regimens that include estrogen used alone—can reactivate or worsen any remaining endometriosis tissue in some patients, so we recommend risk mitigation strategies like combined estrogen-progestogen therapy or close monitoring. Decisions should be personalized based on your symptom burden, imaging findings, and preferences, with multidisciplinary input to balance managing menopausal symptoms against the potential risk of recurrence. When HRT begins, we carefully monitor symptoms and consider follow-up imaging if any concerns arise.
What Are the Key MRI Signs of Malignant Transformation?
The most concerning MRI signs include a new or growing solid mass within an ovarian lesion that lights up with contrast, the disappearance of typical T2 shading, significant restricted diffusion in a solid area, and rapid growth between scans. Any of these findings should prompt a swift evaluation. Correlating these with your clinical exam and tumor markers, along with a timely multidisciplinary discussion for biopsy or surgical excision, are our recommended next steps. Early detection through MRI significantly improves the likelihood of definitive, appropriate management.
How Does MRI Help Manage Pelvic Pain in Postmenopausal Women?
MRI helps us pinpoint pain sources like deep infiltrating nodules, adhesions pulling on organs, and asymmetric masses that explain pelvic pain. This guides targeted interventions, such as excising specific lesions or focused medical therapy. By mapping the location and extent of lesions, MRI allows our surgeons to plan conservative yet comprehensive excisions, reducing the chance of missing disease and improving your pain outcomes. Integrating MRI findings with our multidisciplinary pain management strategies leads to more precise and lasting symptom relief.
- When to consider MRI: If you have persistent, unexplained pelvic pain, an inconclusive ultrasound, suspected deep infiltrating disease, or ovarian masses after menopause.
- What your MRI report will cover: Lesion size, signal characteristics, enhancement pattern, how it relates to your bowel/bladder/ureter, and our suggested level of concern.
- Next steps after a suspicious MRI: A multidisciplinary review, tumor marker assessment if needed, short-interval imaging or targeted biopsy, and surgical planning when appropriate.
These lists clarify practical steps for both clinicians and patients, helping translate MRI findings into actionable management plans and highlighting the crucial role of coordinated care in assessing postmenopausal endometriosis.
Frequently Asked Questions
How does hormone replacement therapy (HRT) fit into managing postmenopausal endometriosis?
Hormone replacement therapy (HRT) can be complex for postmenopausal women with a history of endometriosis. Estrogen used alone might stimulate any remaining endometriosis tissue, potentially raising the risk of recurrence or even cancer. Therefore, a combined estrogen-progestogen regimen is often suggested to help reduce these risks. Your treatment plan will always be personalized, taking into account your symptom severity, imaging results, and personal preferences. Close monitoring and regular follow-ups are vital to ensure HRT doesn’t worsen your endometriosis symptoms.
How can you prepare for an MRI to diagnose postmenopausal endometriosis?
Preparing for an MRI involves several steps to enhance the quality of the images obtained. You might be asked to avoid eating or drinking for a few hours before your procedure. Additionally, bowel preparation, like taking laxatives or following a specific diet, can help us see your pelvic structures more clearly. It’s also important to let our radiology team know about any previous surgeries, allergies, or medical conditions you have. Following these guidelines helps ensure your MRI provides the most accurate diagnostic information possible.
What are the potential complications if postmenopausal endometriosis goes untreated?
If left untreated, postmenopausal endometriosis can lead to several complications, such as ongoing pelvic pain, issues with bowel or bladder function, and the development of adhesions that can impact organ function. There’s also a risk of endometriosis lesions turning cancerous, especially in postmenopausal women. This highlights why timely diagnosis and management are so important, as early intervention can prevent these complications and significantly improve your quality of life. Regular monitoring and imaging are key to managing this condition effectively.
How does our multidisciplinary care benefit you if you have postmenopausal endometriosis?
Multidisciplinary care is essential for managing postmenopausal endometriosis effectively. This approach brings together gynecologists, radiologists, oncologists, and pain management specialists to provide comprehensive care, all tailored to your unique needs. By combining diverse expertise, you receive a holistic treatment plan that addresses not only the physical aspects of endometriosis but also offers emotional and psychological support. This coordinated effort leads to better treatment outcomes, ensures thorough monitoring, and improves your overall satisfaction.
What lifestyle changes can help you manage postmenopausal endometriosis symptoms?
Adopting certain lifestyle changes can help you manage postmenopausal endometriosis symptoms. Regular physical activity can ease pelvic pain and boost your overall well-being. A balanced diet, rich in anti-inflammatory foods like fruits, vegetables, whole grains, and omega-3 fatty acids, can also help reduce inflammation and pain. Stress management techniques, including yoga, meditation, and mindfulness, can further support your symptom relief. Always discuss any lifestyle changes with your healthcare provider to ensure they complement your personalized treatment plan.
What follow-up care do we recommend after treatment for postmenopausal endometriosis?
Follow-up care after treating postmenopausal endometriosis is vital for monitoring your recovery and helping prevent recurrence. You should have regular check-ups to assess how your symptoms are managed and to evaluate any new or persistent concerns. Imaging studies, like MRI, may be recommended periodically to monitor for any changes in endometriosis lesions. Additionally, ongoing discussions about hormone replacement therapy and its effects should be a part of your follow-up visits. This proactive approach helps ensure you receive timely interventions as needed.
Can Endometriosis Be Diagnosed After Menopause?
Yes, endometriosis can persist or even appear for the first time after menopause. Diagnosis relies heavily on imaging like MRI and, when needed, tissue analysis. New symptoms or growing ovarian masses after menopause should prompt a referral to a specialist. In postmenopausal cases, we often see fibrous, non-bleeding lesions that MRI can best characterize, guiding our decision to observe, biopsy, or proceed with excision. Your clinical history—including prior endometriosis, HRT use, and symptom profile—helps us determine the urgency of your care.
Conclusion
Understanding postmenopausal endometriosis and the vital role of MRI in its diagnosis is key to providing you with effective, personalized care. By utilizing advanced imaging techniques, our healthcare providers can accurately identify fibrous lesions and create tailored treatment plans that truly prioritize your well-being. If you’re seeking specialized care, the Endometriosis Center of Excellence offers a comprehensive approach that integrates advanced imaging, expert medical management, and gold-standard surgical options. Schedule a consultation today to explore personalized treatment pathways designed to address your unique needs and bring you lasting relief.

