Gentle, mobility-focused movement, paced and chosen with care, can help people manage endometriosis symptoms. Low-impact activities such as walking, swimming, and Pilates ease pelvic tension, improve circulation, and support mental well‑being. This article summarizes the benefits, safe options, and practical ways to incorporate mobility work into daily life.
Clinical and supervised exercise programs report measurable improvements in quality of life following structured therapeutic regimens for endometriosis.
Key Benefits of Mobility Exercises for Endometriosis
Mobility and low‑impact exercise offer practical, low‑risk ways to address common endometriosis concerns:
- Easing Symptoms: Gentle movement reduces muscle tension and pelvic pain.
- Supporting Hormonal Balance: Regular physical activity supports overall hormonal regulation.
- Improving Blood Flow: Moderate exercise enhances circulation and may lower inflammation.
- Building Pelvic Strength: Low‑load strength and stability protect pelvic structures.
- Enhancing Well‑Being: Consistent activity supports mood and energy.
- Reducing Fatigue: Appropriate movement can counter chronic tiredness.
Tailored mobility work complements medical care and individual tolerance.
Short supervised programs have also reported reductions in pain intensity and improvements in posture.
How Mobility Exercises Help Reduce Pelvic Pain and Inflammation
Mobility work boosts pelvic blood flow, reduces muscle guarding, and supports tissue health without overstretching sensitive areas. Choosing low‑impact options strengthens supporting muscles while minimizing the risk of aggravating lesions, which over time tends to improve pain and daily function.
How Movement Affects Hormones and Mental Health
Regular movement improves sleep, circulation, and stress regulation; endorphin release, breathwork, and mind‑body practices such as yoga help lower stress‑related inflammation and lift mood, complementing medical treatment and resilience-building.
Recommended Gentle Mobility Exercises

Common low‑impact activities recommended for people with endometriosis:
- Gentle Walking – Improves circulation; rest as needed.
- Swimming – Full‑body, low‑impact conditioning.
- Pilates – Builds core control and pelvic stability.
- Stretching – Releases tight muscles and eases cramps.
- Gentle Yoga – Flexibility, breathwork, and relaxation; seek knowledgeable instructors.
Pair activities with rest, hydration, and gradual progression.
Regular, moderate practice that respects personal tolerance is the safest way to progress.
Pelvic Floor and Stretching Exercises That Help
Targeted pelvic‑floor work and gentle stretches support symptoms when performed with relaxation and control; working with a pelvic‑health clinician is recommended to avoid increasing tension.
- Pelvic Floor Relaxation & Controlled Strengthening – Pelvic tilts and gentle, coordinated Kegels instead of forceful squeezes.
- Pilates – Mindful core support.
- Stretching – Slow holds to release tension safely.
- Gentle Yoga – Breath‑integrated movement to ease tightness.
How Yoga and Pilates Support Mobility and Symptom Relief

Yoga and Pilates emphasize controlled movement, breath awareness, and core support—practical strategies that reduce pain sensitivity and help restore mobility when combined with hydration and good nutrition.
Safely Integrating Low‑Impact Workouts Into Your Routine
Practical steps to add low‑impact workouts safely:
- Choose Gentle Options: Start with swimming, walking, Pilates, or stretching.
- Listen to Your Body: Track symptoms and modify movements.
- Balance Activity & Rest: Schedule short recovery breaks.
- Stay Hydrated: Keep fluids regular.
- Consider Complementary Therapies: Gentle yoga, acupuncture, or guided relaxation may help.
- Manage Stress: Use mindfulness and breathing techniques.
These strategies support short‑term comfort and long‑term function.
The Endometriosis Center of Excellence offers personalized care and can help adapt exercise plans to individual needs.
Best Practices for Starting and Maintaining Gentle Exercise Program
Follow evidence‑informed practices when beginning or continuing gentle exercise:
- Favor Low‑Impact Activities: Avoid excess pelvic loading.
- Monitor Your Response: Note what helps or worsens symptoms and adjust slowly.
- Schedule Rest: Planned recovery reduces fatigue.
- Maintain Hydration & Nutrition: Fuel and fluids support energy and healing.
- Add Complementary Practices: Gentle stretching, yoga, or acupuncture as needed.
- Use Stress‑Reduction Techniques: Breathwork and mindfulness for tension management.
- Seek Professional Guidance: Coordinate with gynecologists or pelvic‑health therapists.
These measures promote steady progress and reduce setbacks.
Exercises to Avoid When Managing Symptoms
Avoid high‑impact activities, intense abdominal straining, and moves that sharply increase pelvic pressure; favor controlled, low‑force actions that support healing.
How Mobility Exercises Fit With Treatment and Recovery
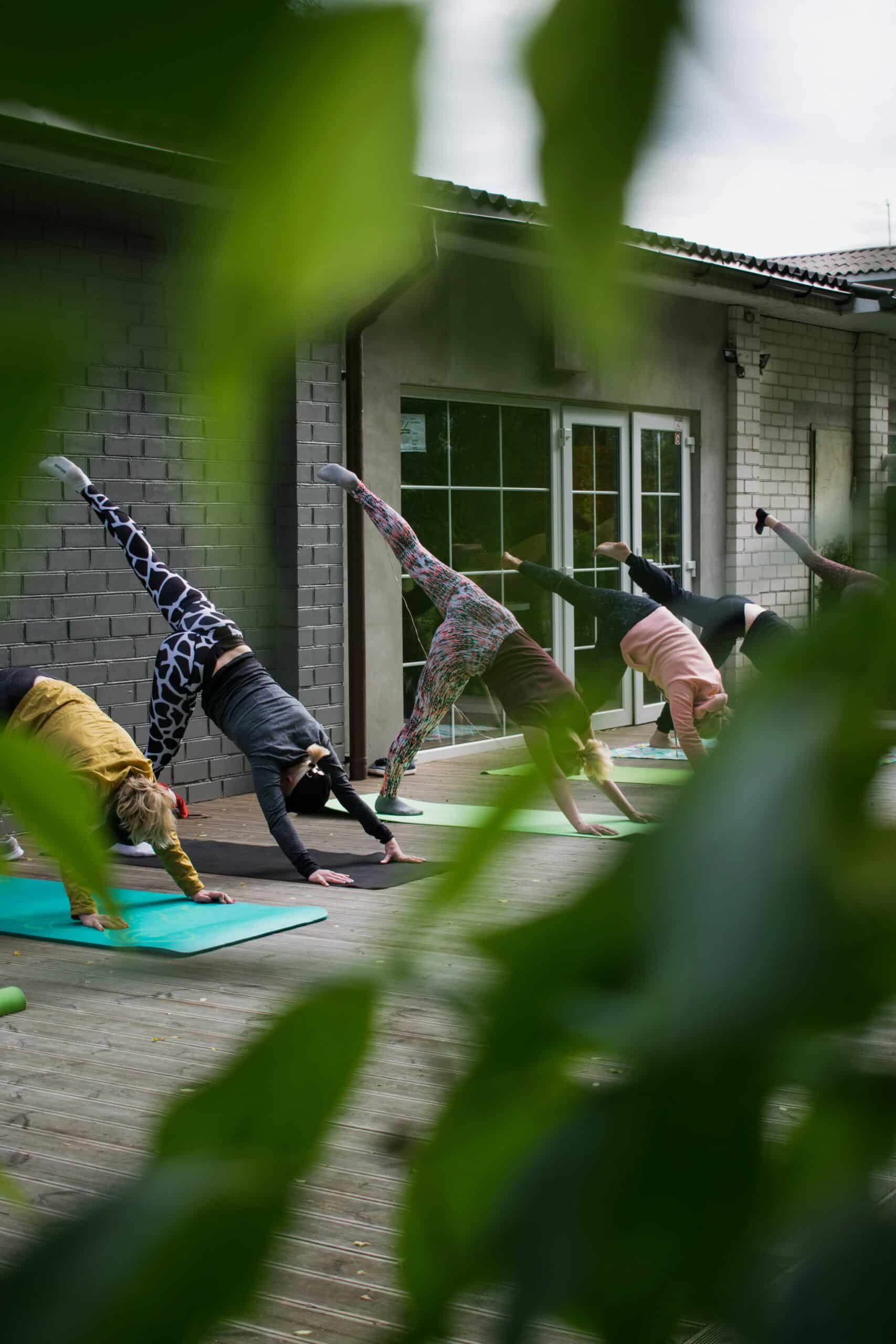
Mobility work complements medical treatments by easing pain, improving circulation, and supporting hormonal and mental‑health goals. Combined with rest, hydration, and appropriate medical care, low‑impact activity forms part of a holistic recovery plan.
Regular movement can be an empowering tool that increases symptom control and improves quality of life.
Frequently Asked Questions
What are the best times to perform mobility exercises for endometriosis?
Choose times when you feel least fatigued or in pain; morning or evening sessions both work, depending on your pattern.
Can I combine mobility exercises with other treatments for endometriosis?
Yes,low‑impact exercise often complements medical care; check with your provider to align plans.
How can I ensure I am performing exercises correctly to avoid injury?
Prioritize form, work with qualified instructors or pelvic‑health therapists, start gently, and progress slowly.
Are there any specific signs that indicate I should stop exercising?
Stop for sharp or severe pain, dizziness, faintness, or persistent nausea; seek professional advice if symptoms continue.
How can I stay motivated to maintain a regular exercise routine?
Set realistic goals, vary activities, track progress, and consider a partner or support group for accountability.
What role does nutrition play in supporting my exercise routine for endometriosis?
Balanced, anti‑inflammatory foods and hydration support recovery and energy; consult a nutritionist for personalized advice.
What types of professionals should I consult before starting mobility exercises for endometriosis?
Consult a gynecologist, pelvic‑health physical therapist, or a fitness professional experienced with pelvic pain for a safe, individualized plan.
How often should I perform mobility exercises to see benefits?
Aim for gentle activity most days, roughly 3–5 short sessions per week, focusing on consistency and gradual increases.
Can mobility exercises help with emotional symptoms related to endometriosis?
Yes. Movement, breathwork, and mind‑body practices release endorphins and reduce stress, which can improve mood and coping.
Are there specific breathing techniques that enhance exercise benefits?
Diaphragmatic (deep belly) breathing and slow rhythmic breathwork promote relaxation and reduce muscle guarding during movement.
What should I do if I feel pain during mobility exercises?
Stop, reassess, and choose a gentler alternative; consult a healthcare professional if pain persists.
How can I track my progress with mobility exercises for endometriosis?
Keep a simple journal of activity type, duration, and symptom levels before and after sessions to monitor changes.
Conclusion
Thoughtfully integrated mobility exercises can meaningfully enhance the quality of life for people living with endometriosis. By adding gentle, consistent movement to daily routines while prioritizing rest, hydration, and professional guidance, patients can strengthen pelvic support, reduce symptoms, and improve emotional well‑being. Begin gradually, adjust as you respond, and explore personalized care options at the Endometriosis Center of Excellence to support your path to relief.

