Endometriosis can cause severe pelvic pain and disrupt daily life. This guide summarizes practical, evidence-informed approaches, non-surgical treatments, lifestyle supports, and surgical options, and explains how the Endometriosis Center of Excellence creates individualized treatment plans to improve comfort and function.
What Are the Main Causes and Types of Endometriosis Pain?

Endometrial-like tissue outside the uterus can trigger ongoing inflammation, which may lead to scarring and adhesions that restrict normal organ movement. Pain can show up as a persistent pelvic ache, severe menstrual cramps, or deep pain with intercourse. Some people also notice pain with bowel movements or urination, especially around their period, along with bloating or fatigue. Paying attention to timing, triggers, and whether symptoms are cyclical or constant helps clarify what’s driving the pain and guides the right treatment approach.
How Does Chronic Pelvic Pain Manifest in Endometriosis Patients?
Chronic pelvic pain often presents as a steady lower-abdominal ache that fluctuates. It can disrupt work and relationships and include sharp flares during menstruation or ovulation that limit daily activities.
What Role Does Inflammation Play in Endometriosis Pain?
Inflammation from ectopic tissue drives swelling and discomfort. Studies show elevated inflammatory markers in many patients, linking inflammation to reported pain and informing targeted therapies.
Which Non-Surgical Strategies Effectively Manage Endometriosis Pain?

Many people experience meaningful symptom relief without surgery through a combination of hormonal treatments, pelvic physical therapy, and complementary therapies. Hormonal options can help suppress lesion activity and reduce inflammation, while pelvic physical therapy addresses muscle tension, nerve sensitivity, and movement restrictions that often contribute to pain. Complementary approaches—such as targeted exercise, pain-modulating techniques, or lifestyle-based support—can further improve daily function. Together, these strategies focus on managing symptoms, improving quality of life, and delaying or avoiding invasive procedures when appropriate.
How Do Hormonal Therapies Help Relieve Endometriosis Pain?
Hormonal treatments (combined contraceptives, progestins, GnRH agonists/antagonists) suppress ovulation or lower estrogen to limit lesion activity. Adjusting hormones often reduces pain, and many patients improve with supervised, consistent use.
Current evidence positions hormonal medical management as a central component of symptom control for many people with endometriosis.
Medical & Hormonal Therapies for Endometriosis Pain
Endometriosis is a common source of pelvic pain in people of reproductive age. Standard medical treatments are primarily hormonal — estrogen–progestin contraceptives, progestins, and gonadotropin-releasing hormone (GnRH) agonists — with other options including androgens and aromatase inhibitors. Emerging roles for GnRH antagonists and selective progesterone receptor modulators are under study. Outside of nonsteroidal anti-inflammatories, nonhormonal drug options (for example, antiangiogenic or immune-modulating agents) need more research. Choosing medical therapy can be complex and should account for side effects, the anatomic type of endometriosis, surgical considerations, current fertility goals, and other pain contributors such as central sensitization. These factors should be discussed individually to ensure tailored treatment and the best possible outcome.
Relating chronic pelvic pain and endometriosis to signs of sensitization and myofascial pain and dysfunction, KJ Heyrana, 2017
What Are the Benefits of Physical Therapy and Complementary Treatments?
Pelvic physical therapy treats pelvic floor dysfunction and myofascial tension to restore mobility and reduce pain. Techniques include myofascial release, targeted stretching, and guided pelvic exercises. Complementary care. acupuncture, mindfulness, relaxation can lower pain perception and support wellbeing.
Recognizing and treating central sensitization and myofascial contributors is often key to relieving persistent pelvic pain when traditional therapies alone fall short.
Endometriosis Pain: Central Sensitization & Myofascial Dysfunction
Chronic pelvic pain can persist despite hormonal or surgical treatments because of changes in the nervous system (central sensitization) and ongoing myofascial dysfunction. Endometriosis may promote neural remodeling that contributes to sensitization and to the formation of painful myofascial trigger points. This work outlines a clinical framework for identifying sensitization and trigger points and reviews targeted treatments — including physical therapy, dry needling, local anesthetic injections, and botulinum toxin — that address myofascial pain directly.
Relating chronic pelvic pain and endometriosis to signs of sensitization and myofascial pain and dysfunction, KJ Heyrana, 2017
At the Endometriosis Center of Excellence we integrate these non-surgical strategies into individualized, multidisciplinary plans aligned with each patient’s goals.
Why Is Endometriosis Excision Surgery Considered the Gold Standard for Pain Relief?
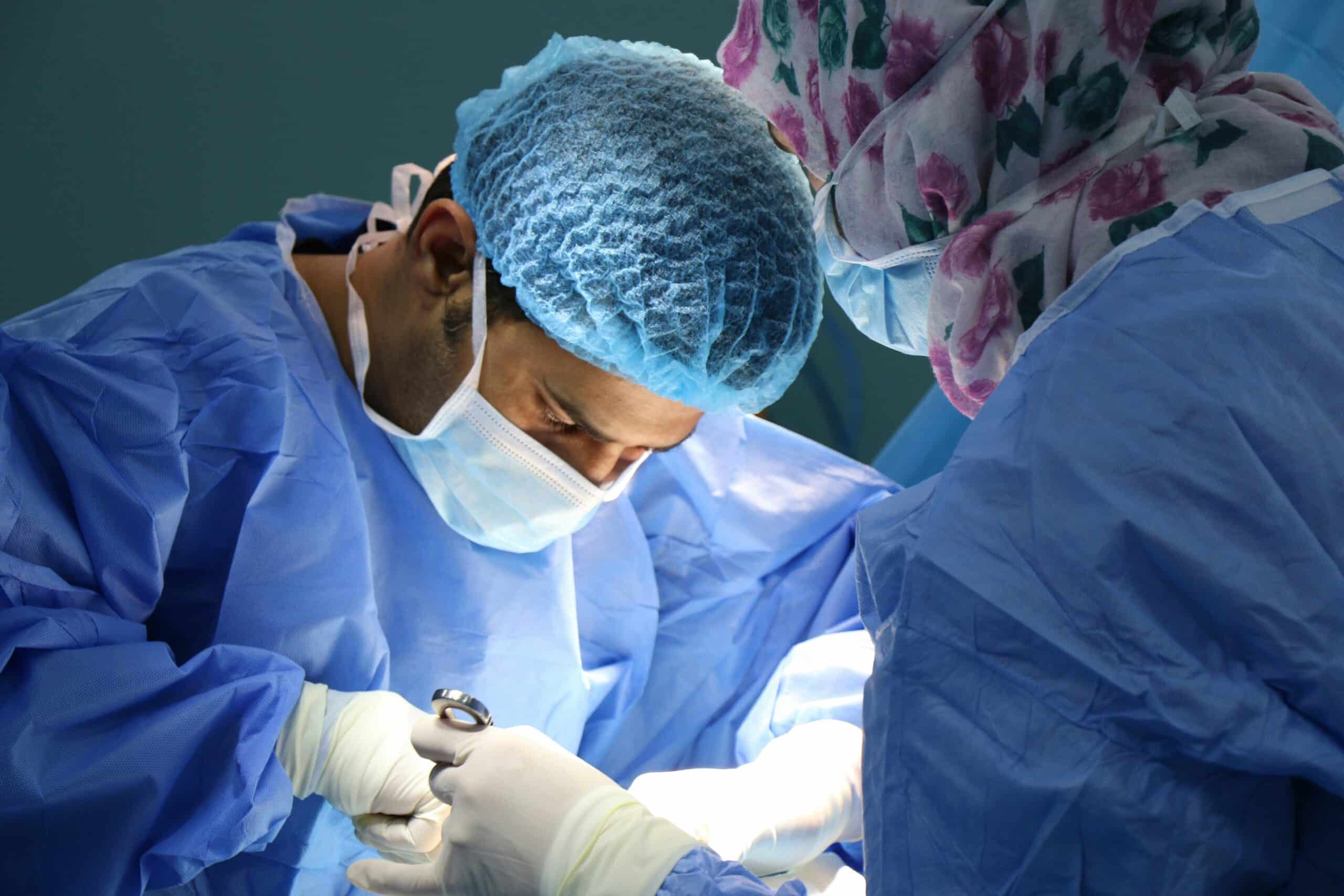
Excision surgery removes endometriosis lesions at their root rather than only treating the surface, which can lead to more durable pain relief for many patients. By fully excising affected tissue, this approach may reduce inflammation and lower the risk of persistent or recurrent symptoms. For people with moderate to severe disease, excision surgery is often associated with meaningful improvements in pain, daily function, and overall quality of life, especially when performed by a surgeon experienced in endometriosis care.
What Are the Benefits and Success Rates of Excision Surgery?
Research shows excision frequently delivers substantial pain relief and sometimes improved fertility. It remains a key option when conservative care fails to control symptoms.
Surgical guidance documents describe the techniques and trade-offs that surgeons consider to maximize pain relief while minimizing risks.
Surgical Management for Endometriosis Pain Relief
Surgical care for patients with chronic pelvic pain should be individualized and multimodal. Laparoscopic excision or ablation is generally preferred over open laparotomy for conservative surgical treatment. Evidence favors cystectomy rather than fenestration or fulguration for endometriomas, though cystectomy can affect ovarian reserve. Procedures such as presacral neurectomy may help those with midline pain, while LUNA has not shown benefit for endometriosis-related pelvic pain. Some surgeons consider appendectomy at the time of pelvic surgery for pain, though more data are needed. In cases of deep infiltrating endometriosis, the potential benefits of aggressive bowel surgery must be balanced against surgical risks.
Surgical management of endometriosis in patients with chronic pelvic pain, 2017
How Does Dr. Rachael Haverland’s Expertise Enhance Surgical Results?
Dr. Rachael Haverland specializes in excision and individualized surgical planning. Her surgeons focus on precise lesion removal while preserving healthy tissue, which many patients report improves symptoms and life quality.
How Can Lifestyle Changes Support Long-Term Endometriosis Pain Relief?

Medical or surgical care often works best alongside lifestyle steps that help lower inflammation and support the body’s overall resilience. Small, sustainable changes—like prioritizing anti-inflammatory, nutrient-dense meals, choosing gentle, consistent movement, and improving sleep—can make symptoms more manageable over time. Stress management also matters, since chronic stress can amplify pain sensitivity and fatigue. Together, these habits can complement treatment by easing symptom flares and improving day-to-day function.
What Anti-Inflammatory Diets Help Reduce Endometriosis Symptoms?
Focus on whole foods: more omega-3s (fatty fish, walnuts, chia), colorful fruits and vegetables, whole grains, and less processed food and sugar. These practical choices may lower systemic inflammation and symptom burden.
How Do Exercise and Stress Reduction Techniques Alleviate Chronic Pain?
Regular gentle exercise and stress-reduction lower pain by improving circulation and releasing endorphins. Yoga, meditation, and guided breathing reduce stress and interrupt pain amplification, supporting function and coping.
The table summarizes common non-surgical approaches, how they work, and typical benefits.
Endometriosis usually needs a layered plan addressing lesions, inflammation, musculoskeletal issues, and emotional health. Combining targeted medical or surgical care with supportive therapies often brings meaningful, lasting relief.
Frequently Asked Questions
What are the common misconceptions about endometriosis pain?
Common myths include that endometriosis only hurts during periods or only affects fertility and long-term reproductive health.. Pain can be chronic and affect bowel or bladder function; better awareness leads to earlier evaluation and treatment.
How can mindfulness and mental health support impact endometriosis pain management?
Mindfulness, CBT, and counseling help manage the emotional impact of chronic pain. These approaches reduce anxiety, change pain perception, and improve daily functioning when used with medical care.
Are there any specific exercises recommended for endometriosis pain relief?
Low-impact activities—walking, swimming, cycling—are generally helpful. Pelvic floor work, targeted stretches, and gentle yoga can reduce pelvic tension. Work with a PT to create a plan that respects pain limits.
What role does the Endometriosis Center of Excellence play in patient care?
The Center provides coordinated, multidisciplinary care — gynecology, pain medicine, pelvic PT, creating individualized plans that consider symptom control and fertility or life goals.
How can support groups benefit those living with endometriosis?
Support groups offer practical tips, emotional validation, and community. Hearing others’ experiences can reduce isolation and suggest coping strategies and resources.
What are the potential side effects of hormonal therapies for endometriosis?
Hormonal treatments may cause weight changes, mood shifts, nausea, altered bleeding, lowered libido, or headaches. Discuss side effects with your clinician to balance benefits and adjust treatment as needed.
Conclusion
Managing endometriosis pain usually requires multiple approaches — medical or surgical care plus lifestyle and emotional support. Working with a specialized, multidisciplinary team helps find sustainable relief. The Endometriosis Center of Excellence offers personalized care; contact them when you’re ready to build a treatment plan to regain comfort and control.

