Pelvic floor therapy can help people with endometriosis lessen pain and regain day‑to‑day function. Below, we explain how targeted physical therapy works, the benefits patients commonly see, and the key techniques clinicians use to address muscle and connective‑tissue contributors to pelvic pain.
Chronic pelvic pain is usually multi‑factorial. Pelvic floor physical therapy is increasingly recognized as an important component of comprehensive care.
Pelvic Floor Physical Therapy for Chronic Pelvic Pain
Chronic pelvic pain (CPP) in women is a complex syndrome linked to sexual dysfunction, musculoskeletal and myofascial disorders, and often psychiatric comorbidity. Because it is common and costly—both in treatment and lost productivity—CPP is a pressing but underrecognized medical need. This systematic review and meta‑analysis evaluated the role of mindfulness and pelvic floor physical therapy (PFPT) in treating or managing women with CPP.
Pelvic floor physical therapy and mindfulness: approaches for chronic pelvic pain in women—a systematic review and meta-analysis, 2023
What Is Pelvic Floor Therapy and How Does It Ease Endometriosis Pain?
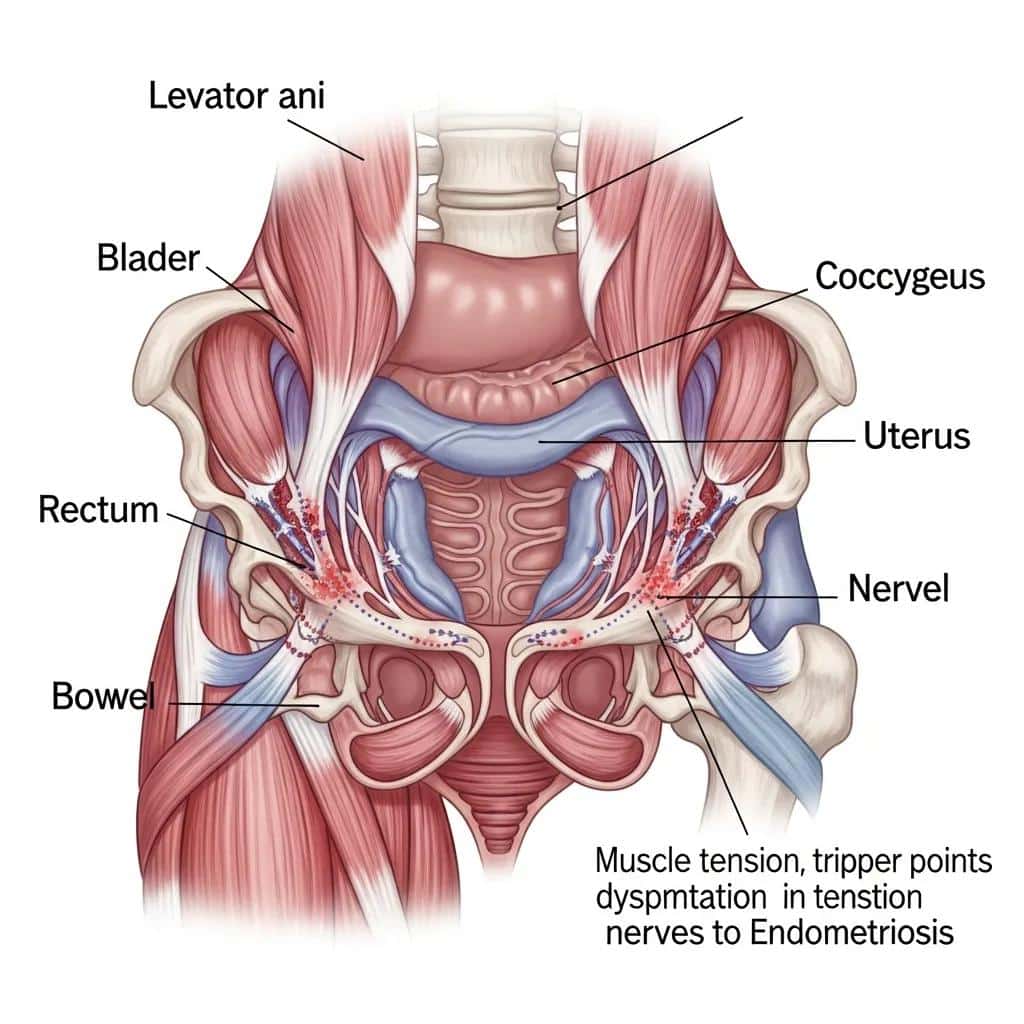
Pelvic floor therapy is a specialized area of physical therapy that focuses on the muscles and connective tissues supporting the bladder, bowel, uterus, and other pelvic organs. Treatment aims to restore balanced strength and relaxation, correcting tension or weakness that can contribute to pain.
By improving muscle coordination, mobility, and relaxation, pelvic floor therapy often reduces endometriosis symptoms such as pelvic pain, pelvic pressure, and pain with activity or intercourse.
Understanding Pelvic Floor Muscles and Their Role in Endometriosis Pain
The pelvic floor muscles support pelvic organs and help coordinate bladder, bowel, and sexual function. When these muscles become tight, weak, or poorly coordinated—often after chronic pain or inflammation—they can amplify discomfort. Identifying and treating these patterns is a key part of recovery.
How Pelvic Floor Therapy Reduces Pain and Restores Function
Therapists combine hands‑on techniques, movement retraining, and relaxation strategies to lower muscle tension, restore normal movement patterns, and teach practical self‑management. Many patients experience meaningful reductions in pain and improved daily function, especially when therapy is integrated with a coordinated care plan.
What Are the Main Benefits of Pelvic Floor Therapy for Endometriosis?
Pelvic floor therapy delivers practical, measurable benefits: less pelvic pain, improved bladder and bowel control, and better overall quality of life.
- Pain relief: Targeted treatment can reduce dysmenorrhea (painful periods) and dyspareunia (painful intercourse) by addressing muscle tension and trigger points.
- Improved bladder and bowel function: Therapy improves pelvic‑floor coordination and strength, easing urgency, pressure, and other functional symptoms.
- Enhanced quality of life: Less day‑to‑day pain often leads to better sleep, more activity, and improved emotional well‑being.
The Endometriosis Center of Excellence in Plano, TX, offers individualized pelvic floor therapy for people with endometriosis. Under the care of Dr. Rachael Haverland, our multidisciplinary team addresses both surgical and non‑surgical contributors to pain.
Pain Relief: Managing Dysmenorrhea and Dyspareunia
Pelvic floor therapy can ease painful periods and pain with intercourse by releasing tight muscles, improving local blood flow, and retraining movement patterns. Many patients report clearer, longer‑lasting relief in these areas.
Improving Bladder and Bowel Function Through Therapy
When endometriosis affects bladder or bowel function, pelvic floor therapy can strengthen and coordinate the muscles that support these systems, helping people regain control and reduce urgency or pelvic‑related dysfunction.
Which Pelvic Floor Therapy Techniques and Exercises Are Used for Endometriosis?
Pelvic floor therapy for endometriosis employs a range of techniques, broadly categorized into manual therapy methods and therapeutic exercises. These approaches work synergistically to address muscle dysfunction, reduce pain, and improve overall pelvic health.
Manual Therapy Methods: Myofascial and Trigger Point Release
Hands‑on methods such as myofascial release and trigger‑point work target tight or restricted tissues to decrease pain, improve range of motion, and normalize muscle behavior.
Addressing myofascial dysfunction and nervous‑system sensitization is especially important because these drivers of pain can persist even after hormonal or surgical treatments.
Physical Therapy for Endometriosis Myofascial Pain
Chronic pelvic pain is a common, frustrating symptom for patients with endometriosis and is often resistant to hormonal and surgical management. While those treatments address ectopic endometrial lesions, they do not directly treat pain from central sensitization or myofascial dysfunction. Myofascial trigger points can continue to generate pain even after standard treatments are optimized. This article outlines how endometriosis may remodel neural networks and contribute to sensitization and trigger‑point formation, presents a clinical framework for identifying these problems, and reviews treatments aimed specifically at myofascial pain—including physical therapy, dry needling, anesthetic injections, and botulinum toxin injections.
Relating chronic pelvic pain and endometriosis to signs of sensitization and myofascial pain and dysfunction, KJ Heyrana, 2017
Therapeutic Exercises: Kegels, Reverse Kegels, and Diaphragmatic Breathing

Exercise and breath work are core parts of therapy. Kegels help build strength, reverse Kegels teach release, and diaphragmatic breathing reduces overall tension. These tools let patients manage symptoms between visits and rebuild confidence in movement.
Who Can Benefit from Pelvic Floor Therapy for Endometriosis Pain Relief?
Pelvic floor therapy offers significant relief and functional improvement for a diverse group of individuals managing endometriosis. It’s particularly beneficial for those exploring non-surgical options, as well as patients preparing for or recovering from excision surgery.
Patients Seeking Non‑Surgical Pain Management Options
Many people with endometriosis prefer non‑invasive approaches. Pelvic floor therapy is a safe, evidence‑based option that targets musculoskeletal contributors without surgical risk.
Integrating Therapy Before and After Excision Surgery
Pelvic floor therapy is helpful both before and after excision surgery. Pre‑operative work prepares tissues and optimizes movement patterns; post‑operative therapy supports healing and reduces the chance of persistent pain, often improving long‑term outcomes.
Evidence supports physical therapy as a valuable part of post‑operative care for improving recovery and limiting ongoing pain after excision.
Pelvic Physical Therapy for Endometriosis Pain
Pelvic physical therapy can be a critical component of post‑operative mobilization. An exercise program designed by a physical therapist may reduce ongoing pain that surgery alone does not eliminate. This study aimed to evaluate the role of exercise in decreasing persistent pain in the post‑excision endometriosis population.
2406 The Role of Exercise in Decreasing Ongoing Pain in the Post‑Excision Endometriosis Population, 2019
Frequently Asked Questions
What should I expect during a pelvic floor therapy session?
Expect a personalized evaluation of pelvic‑floor strength, coordination, and mobility. Sessions typically include hands‑on therapy, guided exercises, breathing practice, and practical education provided in a private, respectful setting.
How long does it take to see results from pelvic floor therapy?
Timing varies. Some people notice improvement after a few sessions; others need several weeks of consistent clinic visits and home practice. Your therapist will set milestones and track progress with you.
Are there any risks or side effects associated with pelvic floor therapy?
Therapy is generally low‑risk. You may feel temporary soreness or mild discomfort; clear communication with your therapist helps tailor techniques for comfort and safety.
Can pelvic floor therapy be combined with other treatments for endometriosis?
Yes. Pelvic floor therapy complements medications, hormonal treatments, and surgery. Coordinating care across your healthcare team usually improves pain management and recovery.
How can I find a qualified pelvic floor therapist?
Ask your gynecologist or primary care provider for referrals, or search for licensed physical therapists with pelvic‑health specialization through professional organizations such as the American Physical Therapy Association (APTA). Look for clinicians experienced in endometriosis and pelvic pain.
Is pelvic floor therapy suitable for men as well?
Yes. Pelvic floor therapy helps people of all genders who have pelvic pain, urinary or bowel concerns, or sexual dysfunction. Therapists tailor treatment to each person’s anatomy and goals.
Conclusion
Pelvic floor therapy is a practical, evidence‑informed option for people with endometriosis who want to reduce pain and improve daily function. By treating muscle and fascial contributors, therapy offers a non‑surgical route to greater comfort and control. Contact our team to discuss a personalized pelvic‑floor plan that supports recovery and long‑term well‑being. Pelvic floor therapy can help people with endometriosis lessen pain and regain day‑to‑day function. Below, we explain how targeted physical therapy works, the benefits patients commonly see, and the key techniques clinicians use to address muscle and connective‑tissue contributors to pelvic pain.