Endometriosis affects a significant number of reproductive-aged women, yet definitive diagnosis often requires surgery and can be delayed by years. Unlocking blood markers for endometriosis diagnosis offers a non-invasive solution that can accelerate care, reduce diagnostic risk, and improve treatment outcomes. In this comprehensive guide, we will define endometriosis and its diagnostic challenges, examine the breakthrough role of biomarkers like CA-125, microRNAs, extracellular vesicles, and emerging protein or genetic indicators, explore the EndoExcellenceCenter’s integrated testing process, survey the latest research propelling personalized diagnostics, and empower patients to access advanced blood test services. By mapping each phase from symptom recognition to specialized consultation, this article clarifies how markers for endometriosis diagnosis can transform patient journeys and foster earlier, more accurate detection.
What Is Endometriosis and How Is It Currently Diagnosed?

Endometriosis is a chronic gynecological condition characterized by endometrial-like tissue growing outside the uterus, causing pain, inflammation, and potential fertility issues. This aberrant tissue follows menstrual cycles, triggers immune responses, and leads to scar formation. Traditionally, diagnosis relies on invasive procedures and imaging studies that often detect disease only after significant progression, underscoring the need for earlier, non-invasive biomarkers.
What Causes Endometriosis and What Are Its Common Symptoms?
Endometriosis arises through mechanisms such as retrograde menstruation, where menstrual blood carrying endometrial cells flows back into the pelvic cavity, genetic predisposition, and immune dysfunction. Hormonal factors, especially estrogen, fuel ectopic tissue growth and sustain chronic inflammation. Common symptoms include:
- Pelvic pain that intensifies during menstruation and may radiate to the lower back or thighs.
- Dysmenorrhea and heavy menstrual bleeding affecting daily activities.
- Infertility or difficulty conceiving due to adhesions and altered pelvic anatomy.
These manifestations often mimic other conditions and delay diagnosis, leading to significant quality-of-life impacts that underscore the urgency of more reliable detection strategies.
How Is Endometriosis Traditionally Diagnosed?
Traditional diagnosis integrates surgical and imaging approaches to identify endometriotic lesions.
Each method confirms endometriosis but carries risks, costs, and potential delays in patient care. Recognizing these constraints highlights the value of blood-based biomarkers for earlier, safer detection.
Why Does Diagnostic Delay Occur and How Does It Affect Patients?
Diagnostic delay in endometriosis averages seven to ten years due to symptom overlap with other disorders, limited specialist access, and reliance on surgery for confirmation.
- Misattribution of pelvic pain to menstrual cramps or gastrointestinal issues leads to repeated consultations.
- Hesitancy to undergo invasive procedures prolongs clinical evaluation.
- Insurance and referral barriers extend wait times for specialist imaging or laparoscopic evaluation.
Prolonged delay exacerbates pain, fertility impairment, and emotional distress, reinforcing the need for non-surgical diagnostic alternatives that can close the gap between symptom onset and effective care.
Why Are Blood Markers a Breakthrough for Non-Invasive Endometriosis Diagnosis?
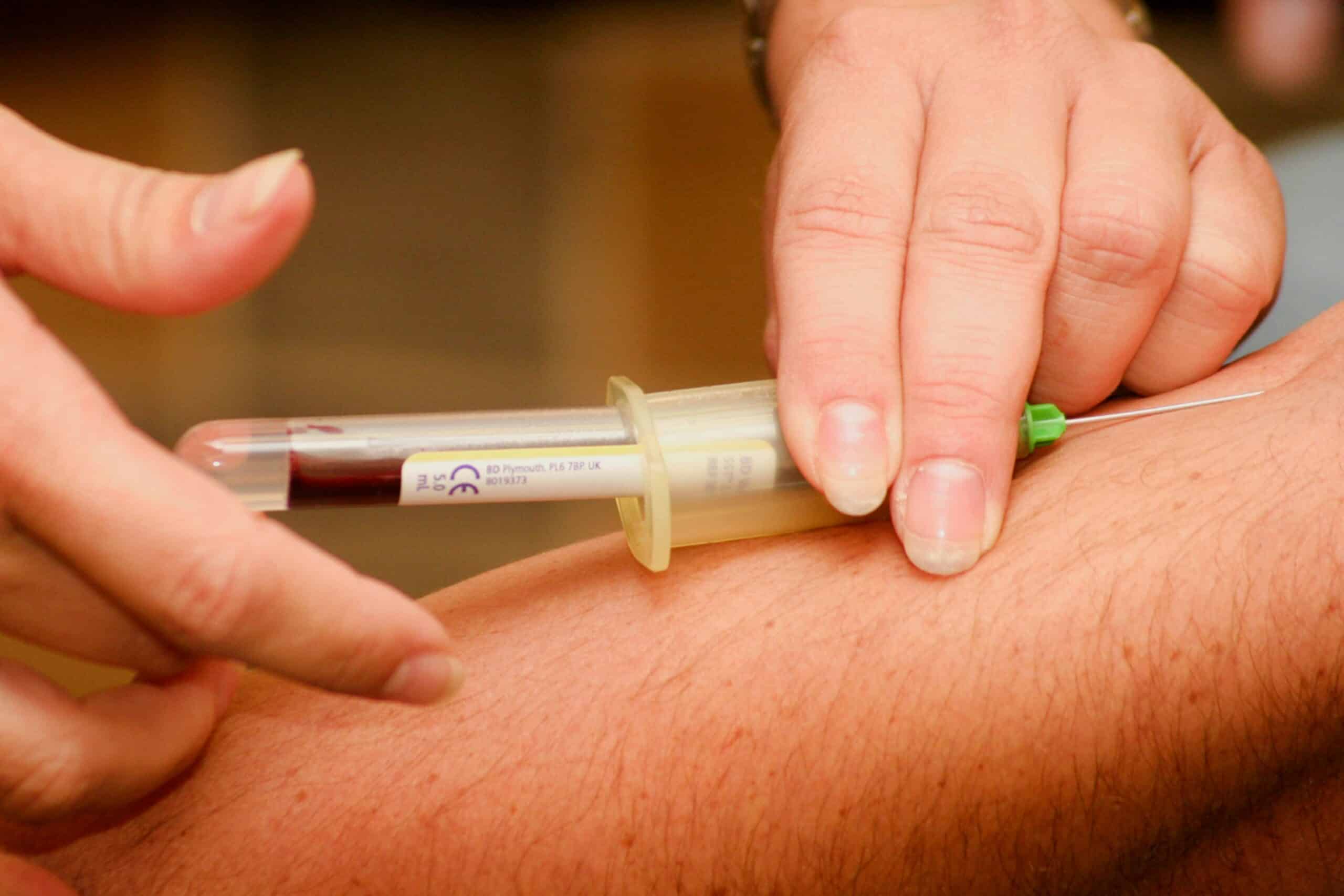
Blood markers represent measurable substances in serum or plasma that correlate with endometriotic activity, inflammation, or tissue remodeling. By detecting specific biomolecules, these tests enable earlier and less risky disease detection compared to surgical or imaging methods. This non-invasive approach aligns with patient preferences and clinical goals for timely, accurate diagnosis.
What Are the Limitations of Current Diagnostic Methods?
Conventional diagnostic tools for endometriosis face challenges in safety, accuracy, and accessibility:
- Invasiveness: Laparoscopic confirmation requires surgery under general anesthesia.
- Sensitivity: Imaging techniques may miss deep infiltrating or small lesions.
- Delay: Specialist referrals and procedural scheduling cause months-long wait times.
Such obstacles drive the search for biomarkers that can be measured in a simple blood draw, overcoming the practical barriers of existing methods and opening the door to wider early screening.
How Do Blood Markers Enable Early and Safer Detection?
Blood markers function by revealing biological signatures of endometriosis through detectable changes in protein levels, nucleic acid fragments, or cell-derived particles. These tests:
- Identify systemic inflammation and aberrant cell signaling before macroscopic lesions appear.
- Allow repeat monitoring to assess disease progression or treatment response.
- Eliminate surgical risks, anesthesia complications, and prolonged recovery.
By translating molecular insights into clinical tools, blood markers shift diagnosis from invasive confirmation to proactive detection.
What Are the Key Benefits of Using Blood Tests for Endometriosis?
- Reduced Risk: Eliminates procedural complications associated with laparoscopy and imaging contrast agents.
- Faster Diagnosis: Yields results within days, enabling earlier intervention.
- Patient Comfort: Meets patient preference for non-invasive testing and minimizes treatment avoidance.
- Cost Efficiency: Cuts down surgical and imaging expenses through targeted screening.
These benefits underscore how blood markers revolutionize the diagnostic pathway, paving the way for improved outcomes and personalized management.
Which Blood Markers Are Used for Endometriosis Diagnosis?

Diagnosing endometriosis has long been a challenge, often requiring invasive procedures like laparoscopy to confirm the condition. In recent years, however, researchers have been investigating blood-based biomarkers as a less invasive way to aid in diagnosis. While no single marker has yet proven definitive, several have shown promise in signaling the presence of endometriosis. These include CA-125, one of the earliest studied markers, along with emerging candidates such as CA 19-9, interleukins, tumor necrosis factor-alpha (TNF-α), vascular endothelial growth factor (VEGF), and microRNAs. Understanding which blood markers are under investigation, how they work, and their current limitations can help patients and providers alike gain clarity on where science stands today, and what this could mean for earlier, more accurate detection in the future.
What Is CA-125 and What Are Its Strengths and Limitations?
CA-125 provides a useful initial screen but requires combination with additional markers to improve specificity and reduce false positives, leading naturally to testing of nucleic acid and vesicle-based indicators.
How Are MicroRNAs Emerging as Promising Endometriosis Biomarkers?
MicroRNAs are short, non-coding RNA sequences that regulate gene expression and are released into circulation during disease processes.
- Differential expression patterns of miR-20a, miR-143, and miR-451 have been linked to endometriotic lesion activity.
- Circulating microRNA panels demonstrate higher specificity than single protein tests.
- Stability in blood samples allows reliable detection across laboratories.
These features position microRNAs as powerful diagnostic tools that can be integrated into multi-marker blood panels for enhanced accuracy.
What Role Do Extracellular Vesicles Play in Diagnosis?
Extracellular vesicles (EVs) are membrane-bound particles shed by cells carrying proteins, RNAs, and lipids reflective of tissue origin.
- Endometrial stromal cell-derived EVs exhibit unique surface proteins and cargo linked to inflammation and angiogenesis.
- EV isolation and analysis reveal disease-specific signatures not captured by free-circulating markers.
- EV-based assays can differentiate endometriosis from other pelvic pain etiologies.
The diagnostic value of EVs lies in their encapsulated molecular detail, offering a window into lesion biology and complementing protein or RNA markers.
What Other Protein and Genetic Markers Show Potential?
- Interleukin-6 (IL-6) – Proinflammatory cytokine elevated in endometriosis serum.
- VEGF (Vascular Endothelial Growth Factor) – Reflects lesion-driven angiogenesis.
- KRAS Mutations – Somatic alterations identified in endometriotic tissues.
Combining these protein and genetic markers into an integrated panel can enhance diagnostic accuracy and support personalized risk stratification.
How Do Endo Centers Use Blood Markers in Its Diagnostic Process?

Patients undergo a routine blood draw processed through specialized laboratory protocols:
- Sample Collection – Standard venipuncture during clinical consultation.
- Biomarker Panel Analysis – Multiplex assays measure CA-125, select microRNAs, and EV profiles.
- Quality Control – Internal standards verify assay accuracy and reproducibility.
This streamlined procedure prioritizes patient comfort and delivers results within 5–7 business days, enabling rapid follow-up.
How Are Blood Test Results Interpreted for Accurate Diagnosis?
Interpreting results involves correlating biomarker levels with clinical indicators:
- Elevated CA-125 and IL-6 prompt imaging referrals to localize lesions.
- Distinct microRNA signatures modulate suspicion levels for superficial versus deep-infiltrating disease.
- EV profiles guide risk assessment and surgical planning when necessary.
By contextualizing molecular data alongside symptoms and imaging, clinicians achieve a holistic diagnostic picture that informs personalized care.
How Are Blood Markers Combined with Other Diagnostic Tools?
- Symptom Assessment → standardized pain and quality-of-life questionnaires.
- Blood Marker Screening → non-invasive molecular profiling.
- Targeted Imaging → ultrasound or MRI reserved for high-risk or equivocal cases.
- Minimally Invasive Confirmation → laparoscopy considered when biomarker and imaging results conflict.
This tiered strategy minimizes unnecessary procedures while maximizing diagnostic confidence and patient safety.
What Are the Latest Advances and Future Directions in Endometriosis Blood Marker Research?

For decades, CA-125 hinted at endometriosis but fell short as a standalone diagnostic. Today, the field is shifting toward panel-based biomarkers and multi-omics, combining proteomics, metabolomics, and microRNA profiles, with machine-learning classifiers to boost accuracy and detect disease across stages. Researchers are also exploring non-invasive specimens like menstrual effluent, saliva, and plasma (including extracellular vesicles and cell-free DNA) to reduce reliance on surgery. Early studies suggest these signatures may track disease activity, phenotype, and treatment response, opening the door to monitoring tools and point-of-care tests.
Still, progress hinges on large, diverse cohorts, standardized sample handling, and rigorous external validation to avoid overfitting and bias. This article reviews the latest advances in blood-based markers and maps the near-term roadmap, from discovery pipelines to clinically usable assays that could finally shorten time to diagnosis and personalize care.
What Clinical Trials Are Exploring New Blood Markers?
- A trial assessing a combined microRNA/EV signature in adolescents with chronic pelvic pain.
- Studies investigating proteomic biomarkers like annexin A2 for early lesion detection.
- Comparative trials of biomarker-guided versus standard diagnostic pathways measuring time-to-diagnosis and patient outcomes.
Results from these trials will validate new markers and support regulatory approval for broader clinical use.
How Will Personalized Medicine Change Endometriosis Diagnosis?
- Genetic risk factors (e.g., KRAS variants) combined with biomarker levels to stratify candidates for early testing.
- Dynamic biomarker monitoring to assess treatment response and predict recurrence.
- Integration of electronic health records and molecular data using machine-learning algorithms for precision risk prediction.
These advances will enable truly individualized diagnostic pathways that adapt to each patient’s biology and clinical context.
What Emerging Technologies Could Improve Diagnostic Accuracy?
- Digital PCR – Ultra-sensitive detection of low-abundance nucleic acids.
- Single-EV Profiling – Characterization of individual vesicles for finer-scale signatures.
- Artificial Intelligence – Pattern recognition across complex multi-marker datasets.
By harnessing these technologies, the next generation of blood tests will deliver unprecedented specificity and sensitivity, further reducing reliance on invasive procedures.
What Should Patients Know About Blood Tests for Endometriosis?
Blood tests are often part of the diagnostic process when doctors suspect endometriosis, but their role can sometimes be misunderstood. Unlike conditions with a single definitive blood marker, endometriosis is more complex, and no single test can provide a clear diagnosis on its own. Instead, blood tests may help rule out other conditions, identify signs of inflammation, or measure certain biomarkers that support a broader clinical evaluation. For patients navigating symptoms like pelvic pain, fatigue, or fertility challenges, understanding what blood tests can, and cannot, reveal is an important step in managing expectations and making informed decisions about next steps in care.
Can Endometriosis Be Diagnosed Without Surgery Using Blood Tests?
Yes, while laparoscopy remains definitive, advanced blood marker panels provide high-confidence, non-invasive diagnostic alternatives. Comprehensive assays combining CA-125, microRNAs, and EV profiles can achieve sensitivity and specificity levels that guide clinical decision-making and may obviate surgery in clear-cut cases.
How Accurate and Reliable Are Blood Marker Tests?
Diagnostic accuracy varies by marker panel composition and disease stage:
- Single markers like CA-125 show moderate sensitivity.
- Multi-marker panels including microRNAs and EVs report specificity upwards of 80–90%.
- Ongoing validation studies continue to refine cutoff values and performance metrics.
Reliability improves when molecular results are interpreted alongside clinical evaluation and imaging, ensuring a balanced diagnostic assessment.
When Should Patients Consider Blood Marker Testing?
- Experiencing persistent pelvic pain unresponsive to standard therapies.
- Facing fertility challenges with suspected endometriosis etiology.
- Seeking a less invasive diagnostic option before imaging or surgery.
Discussing blood-based screening with a specialist can clarify timing and appropriateness based on individual health status and family history.
Conclusion
Utilizing blood markers for endometriosis diagnosis offers a groundbreaking, non-invasive approach that can significantly reduce diagnostic delays and improve patient outcomes. By integrating biomarkers like CA-125 and microRNAs, healthcare providers can achieve earlier detection and personalized treatment strategies. This innovative method not only enhances patient comfort but also aligns with the growing demand for safer diagnostic alternatives. To learn more about how these advancements can benefit you or your patients, explore our resources today.

