Endometriosis can cause persistent pelvic pain and disrupt daily life. This guide explains how physical therapy — a non-surgical, evidence-informed approach — can help reduce pain, restore function, and assist people in returning to their usual activities. You’ll find clear descriptions of how therapy works, practical exercises, and how therapists support recovery after excision surgery.
How Does Physical Therapy Alleviate Endometriosis Pain?

Physical therapy targets the musculoskeletal contributors to pelvic pain. Hands‑on care, manual therapy, and tailored exercise ease muscle tension, improve pelvic floor coordination, and restore mobility. Addressing these factors can lower pain and make daily tasks easier.
Clinical studies and case reports increasingly highlight the role of physical therapy in treating persistent pelvic pain and pelvic floor dysfunction related to endometriosis.
Evidence and patient reports show that people who engage in physical therapy often have reduced chronic pelvic pain and better function.
What Physical Therapy Techniques Target Pelvic Floor Dysfunction?
Common techniques include myofascial release to ease fascial and muscle restrictions, pelvic floor muscle training (PFMT) to strengthen and coordinate the pelvic muscles, and manual therapy to improve tissue mobility. These approaches are combined to help manage symptoms and improve body control.
How Does Manual Therapy Reduce Muscle Tension and Trigger Points?
Manual therapy releases localized tightness and trigger points, restoring circulation and range of motion. Targeted pressure and movement reduce guarding and improve tissue extensibility, and many patients report better pain and movement after a comprehensive endometriosis treatment approach paired with exercise and education.
Which Physical Therapy Exercises Are Best for Endometriosis Symptoms?

A balanced program blends strength, flexibility, and relaxation. Exercises support the pelvic floor, relieve surrounding muscle strain, and lower pain sensitivity.
- Pelvic Floor Exercises
PFMT (including properly performed Kegels) restores strength and coordination and can reduce pelvic pressure and pain. - Stretching Techniques
: Gentle stretches for the hips, groin, and lower back relieve tightness that contributes to discomfort. - Breathing Techniques
: Diaphragmatic breathing and relaxation lower muscle tension and help during flare‑ups.
These recommendations align with studies that describe comprehensive programs combining strength, flexibility, and relaxation components.
What Are Effective Pelvic Floor Exercises for Endometriosis Relief?
PFMT — when done correctly and regularly — improves support and can reduce pelvic pain. A simple approach:
- Identify the pelvic floor by briefly and safely stopping urine flow to feel the muscles (only to locate them, not as regular exercise).
- Contract for about 5 seconds, then relax for 5 seconds.
- Repeat 10–15 times per set, aiming for three short sessions spread throughout the day.
Supervision by a therapist ensures the correct technique and promotes better long-term pelvic health.
How Do Stretching and Breathing Techniques Support Symptom Management?
Stretching helps reduce tightness in the pelvis, hips, and lower back. When combined with diaphragmatic breathing, stretching promotes relaxation, lowers nervous system arousal, and reduces pain sensitivity. A few minutes of slow, deep breathing daily can help make flare‑ups more manageable.
How Is Physical Therapy Integrated with Endometriosis Excision Surgery Recovery?
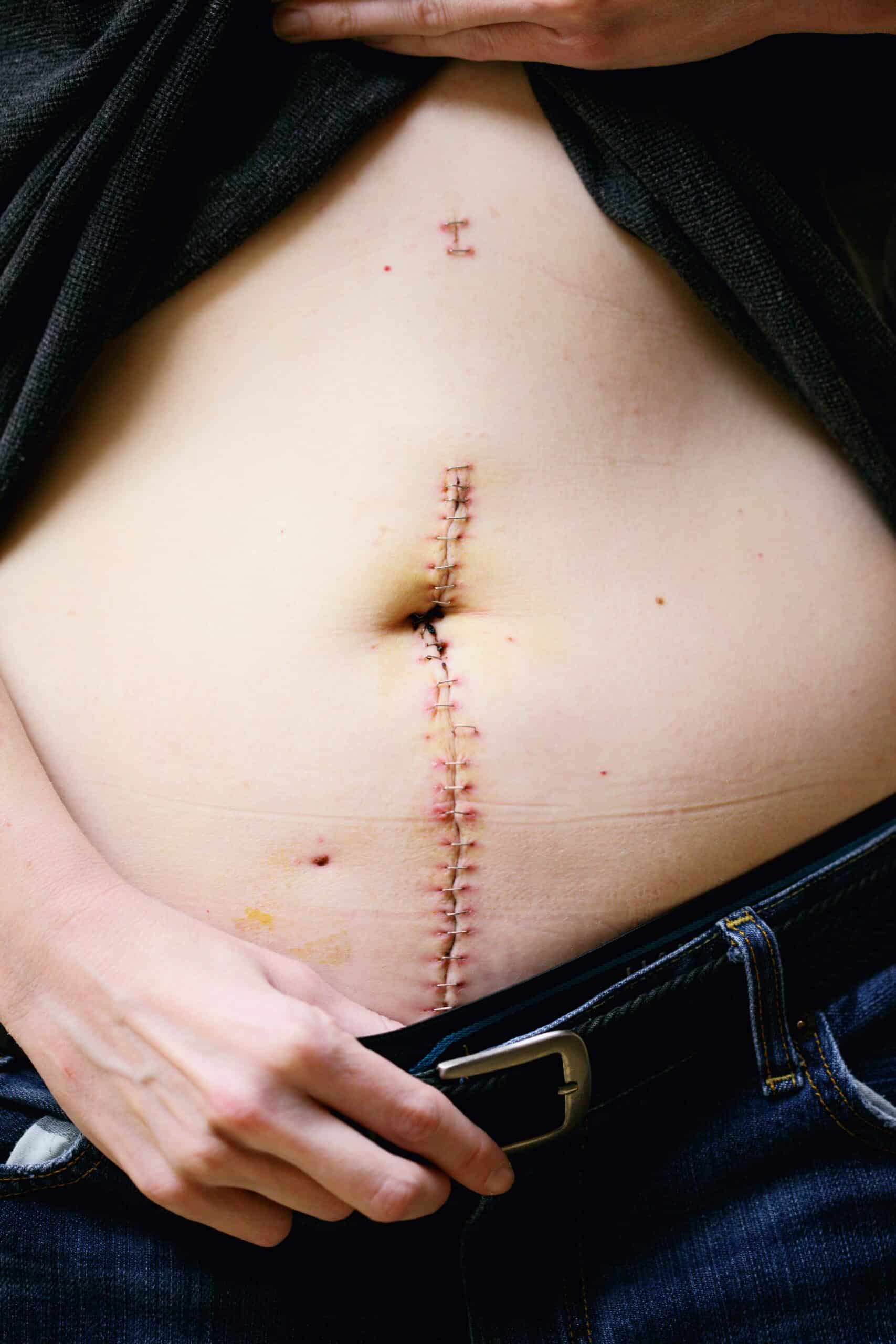
Physical therapy supports recovery both before and after excision. Coordinated care with your surgical team can speed rehabilitation and reduce postoperative pain and dysfunction.
Pre-surgical work emphasizes strength and mobility, thereby preparing the body more effectively for surgery, which can facilitate a smoother rehabilitation process.
Post-surgical therapy focuses on a safe return to activity, scar and soft-tissue mobilization, progressive strengthening, and pain management to help patients regain function more quickly.
What Role Does Pre‑Surgical Physical Therapy Play in Preparation?
Pre-surgical therapy enhances pelvic floor control, core and hip strength, and flexibility, thereby creating a stronger foundation for recovery.
How Does Post‑Surgical Physical Therapy Enhance Recovery and Function?
Post-surgical plans progress from gentle movement to full activity, addressing scar mobility, strength, coordination, pacing, and pain management to facilitate a safer, faster return to daily life.
What Are the Emotional and Quality of Life Benefits of Physical Therapy for Endometriosis?

Physical therapy can restore confidence, provide practical symptom‑management tools, and often improve mood, reduce anxiety, and increase participation in work and relationships.
Many people also report better mental well-being after starting a consistent therapy plan because they feel supported and understood by pelvic‑health clinicians.
How Does Physical Therapy Support Mental Well‑Being in Endometriosis Patients?
A trusting therapist‑patient relationship creates a safe space for emotional concerns. Therapists teach techniques such as pacing, relaxation, and coping skills that reduce stress and improve sleep — all of which are essential for maintaining mental health.
What Improvements in Daily Function and Comfort Can Patients Expect?
With consistent therapy, people often notice improved mobility, less pain with daily tasks, and greater ease with exercise and intimacy. Over time, this leads to improved fitness, enhanced self-management, and increased resilience.
The table summarizes common pelvic physical therapy techniques and supporting evidence.
Together, these methods create a patient‑centered approach to managing endometriosis by addressing physical contributors to pain and supporting emotional recovery.
Frequently Asked Questions
What should I expect during my first physical therapy session for endometriosis?
Expect a detailed history, symptom review, and a physical assessment of movement, posture, and pelvic floor function as appropriate. Your therapist will propose a personalized plan with realistic short‑ and long‑term goals.
How often should I attend physical therapy sessions for optimal results?
Frequency depends on needs. Many start with one to two sessions per week, then taper as they progress. Your therapist adjusts the plan based on response and goals.
Can physical therapy be combined with other treatments for endometriosis?
Yes. Physical therapy complements medications, hormonal treatments, and surgery. Coordinated care can enhance recovery and long‑term function — discuss combinations with your medical team.
Are there any risks or side effects associated with physical therapy for endometriosis?
Physical therapy is generally safe. Temporary soreness after new exercises or techniques is common. A thorough assessment helps tailor care and reduce risks; techniques are modified if needed.
How long does it typically take to see improvements from physical therapy?
Timelines vary. Some notice changes in a few sessions, while others require weeks or months of consistent work. Severity, adherence, and individual healing affect pace.
What lifestyle changes can complement physical therapy for endometriosis relief?
Minor adjustments can help: prioritize anti-inflammatory foods, stay hydrated, engage in gentle regular activity, and practice stress-reducing habits like yoga or mindfulness. A symptom diary can clarify triggers and progress.
Conclusion
Physical therapy offers a practical, patient‑centered way to reduce pain and improve function for people with endometriosis. Through tailored exercises, hands‑on care, and education, therapy supports physical recovery and emotional well-being. If you’re ready to explore individualized, evidence‑informed care, our pelvic health programs are designed to help you move and live with less pain.

