Endometriosis affects millions of women worldwide, causing pelvic pain, heavy bleeding, and fertility issues. Women face multiple treatment options depending on disease severity, age, and overall health. This article compares treatment modalities—hormonal therapies, surgical procedures, pain management, complementary methods, and lifestyle changes—to empower patients with clear, evidence-based guidance for informed decision-making. It also touches on emerging therapies and ongoing research that continue to shape endometriosis care.
Key Takeaways
- Endometriosis treatment includes hormonal therapies, surgical procedures, pain management, complementary therapies, and lifestyle modifications.
- Hormonal treatments (e.g., birth control pills, GnRH agonists) reduce lesion growth and pain, but carry side effects.
- Surgical options like laparoscopy and hysterectomy provide relief for advanced cases, though recovery and risks vary.
- Complementary therapies and lifestyle changes, including acupuncture and dietary modifications, can enhance overall outcomes.
- Emerging research promises more personalized and effective approaches.
What Are the Main Treatment Options for Endometriosis?

Endometriosis treatment aims to address multiple aspects of the condition—minimizing inflammation, slowing the growth of endometrial lesions, managing chronic pain, and ultimately enhancing overall quality of life. A range of options is available to support these goals, including:
How Do Hormonal Therapies Work for Endometriosis?
Hormonal treatments lower estrogen levels—which fuel endometrial growth—by inducing a hormone-stable or hypoestrogenic state. Medications such as birth control pills, progestins, GnRH agonists, and danazol reduce menstrual flow and lesion size. They relieve pain in many patients (with reported relief in 60–80% of cases), although side effects like mood changes, weight gain, and decreased bone density require monitoring.
What Pain Management Strategies Are Available?
Pain is managed using NSAIDs, which reduce inflammation and relieve cramping. In cases of severe pain, opioids may be used briefly, although their risk of dependency limits long-term use. Adjunct techniques—such as physical therapy and cognitive-behavioral therapy—help reduce pain intensity and improve daily functioning when combined with medications.
When Is Surgery Recommended for Endometriosis?
Surgical intervention is considered when medical therapy fails or the disease is advanced. Laparoscopy, a minimally invasive procedure, removes lesions and adhesions, offering significant pain relief (up to 70% of patients) and improving fertility. In extensive cases, more radical options such as hysterectomy (often with ovary removal) may be necessary, though these carry higher risks, including infection and longer recovery times.
What Complementary Therapies Can Support Endometriosis Treatment?
Complementary therapies such as acupuncture, herbal remedies, and mind-body practices support conventional treatment. Acupuncture may lower pain scores by 20–30% by improving blood circulation and triggering endorphin release. Herbal options (e.g., turmeric, ginger) may reduce inflammation, while yoga and mindfulness help relieve stress, contributing to overall emotional well-being.
How Can Lifestyle Modifications Improve Endometriosis Symptoms?
Lifestyle changes are vital. Regular exercise increases endorphin levels and reduces stress hormones, contributing to a 25–40% improvement in pain and fatigue. A diet rich in anti-inflammatory foods (fruits, vegetables, omega-3 fatty acids) and low in processed foods helps manage inflammation. Stress management through meditation, deep breathing, and proper sleep further supports symptom control.
How Do Hormonal Therapies Compare for Treating Endometriosis?

Hormonal therapies vary in how they work, their effectiveness, and the side effects they may cause. Understanding these differences is key to choosing the most suitable option for managing endometriosis symptoms.
What Are the Benefits and Risks of Birth Control Pills?
Birth control pills combine estrogen and progestin to regulate menstrual cycles, reduce flow, and suppress ovulation, leading to decreased endometrial activity and pain reduction (up to 50% improvement). However, they carry risks such as blood clots, weight gain, and mood fluctuations.
How Effective Is Progestin Therapy for Endometriosis?
Progestin therapy mimics natural progesterone, discouraging endometrial growth. It is available as pills, injections, or IUDs and can reduce pain by 40–60% over several months. Its benefits include fewer estrogen-related side effects, though breakthrough bleeding and potential bone health issues may occur with long-term use.
What Should You Know About GnRH Agonists?
GnRH agonists dramatically lower estrogen by inducing a temporary menopausal state, leading to up to a 70% reduction in pain. They may cause menopausal symptoms (hot flashes, vaginal dryness, and bone density loss), which are often managed with low-dose hormone add-back therapy.
When Is Danazol Used and What Are Its Side Effects?
Danazol, a synthetic androgen, suppresses estrogen production by acting on the hypothalamic-pituitary-ovarian axis. While effective at reducing pain and lesion size, its androgenic side effects (e.g., weight gain, acne, unwanted hair growth) limit its long-term use. It is typically reserved for patients who cannot tolerate other hormonal options.
What Are the Surgical Treatment Options and Their Outcomes?
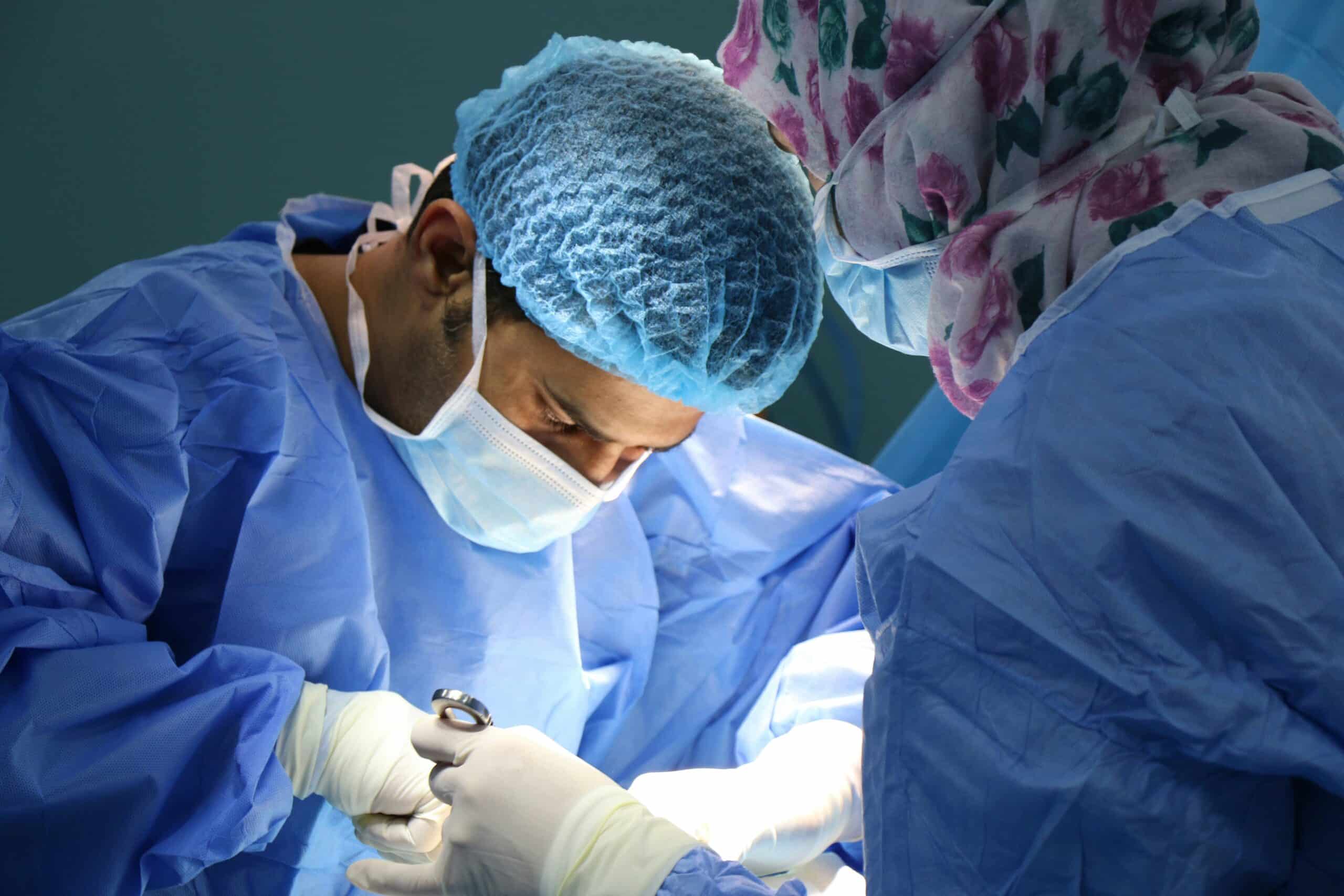
Surgical treatments differ in their level of invasiveness, effectiveness, and recovery time, each offering unique benefits depending on the severity and goals of care.
How Does Laparoscopy Treat Endometriosis?
Laparoscopy, using small incisions, allows surgeons to remove or ablate endometrial lesions. It can produce long-term relief in 60–70% of patients and may improve fertility. However, recurrence is possible, sometimes necessitating repeat procedures.
When Is Hysterectomy Considered for Endometriosis?
Hysterectomy is generally reserved for severe cases in women who have completed childbearing. It may include removal of the ovaries to decrease estrogen production. Though it can provide permanent relief from symptoms, the procedure carries significant risks and may lead to surgical menopause.
What Are the Risks and Recovery Expectations of Surgery?
All surgeries carry risks such as bleeding, infection, and injury to nearby tissues. Laparoscopic recovery typically spans 2–4 weeks, while more extensive surgeries may require months of recovery. Postoperative care, including pain management and rehabilitation, is essential to prevent recurrence and ensure optimal outcomes.
Which Pain Management Techniques Are Most Effective for Endometriosis?

Managing pain is one of the most critical aspects of living with endometriosis, as it can significantly impact daily functioning and emotional well-being. From medications to lifestyle changes and alternative therapies, a variety of pain management strategies are available. Understanding which techniques are most effective can help patients find lasting relief and regain control over their lives.
How Do NSAIDs Help Manage Endometriosis Pain?
NSAIDs decrease inflammation and reduce the production of prostaglandins, helping to alleviate cramping and pain by 30–50%. They are affordable and work rapidly, though gastrointestinal side effects and long-term kidney concerns must be considered.
When Are Opioids Prescribed and What Are the Concerns?
Opioids are reserved for severe pain that does not respond to other treatments. They provide potent relief by binding to opioid receptors, but risks such as dependency, tolerance, sedation, and constipation limit their use to short-term or multimodal strategies.
What Other Pain Management Approaches Are Available?
Additional techniques include physical therapy, nerve blocks, and cognitive-behavioral therapy, which can improve pelvic muscle function and reduce pain signals. Holistic approaches like acupuncture complement these methods by modulating nerve activity and inflammation.
How Can Complementary Therapies Enhance Endometriosis Treatment?
Complementary treatments help reduce side effects and improve overall well-being:
What Role Does Acupuncture Play in Symptom Relief?
Acupuncture stimulates specific body points with fine needles to improve blood circulation and trigger endorphin release. Studies suggest it can lower pain by 20–30%, making it a safe adjunct to medical treatment.
Are Herbal Remedies Effective for Endometriosis?
Herbal remedies such as turmeric, ginger, and cinnamon may possess anti-inflammatory and analgesic properties. Though evidence is limited, these natural agents can reduce pain and inflammation by 15–25% when used under professional guidance.
How Does Diet Influence Endometriosis Symptoms?
A balanced diet rich in fruits, vegetables, whole grains, and omega-3 fatty acids helps reduce inflammation and improve hormone regulation. Limiting red meat and processed foods can further decrease inflammatory markers, contributing to symptom relief.
What Lifestyle Changes Can Support Endometriosis Management?

Lifestyle changes can play a powerful role in managing endometriosis symptoms, complementing medical treatments and improving overall well-being.
How Does Exercise Affect Endometriosis Symptoms?
Regular, moderate exercise improves circulation, boosts endorphin levels, and reduces stress, leading to a 25–40% improvement in pain and fatigue. Activities such as yoga, Pilates, and aerobic exercises also aid in maintaining flexibility and overall fitness.
What Stress Management Techniques Are Recommended?
Techniques like mindfulness meditation, deep breathing, and progressive muscle relaxation lower cortisol levels and reduce inflammation. These practices can improve sleep quality and overall well-being, helping to alleviate pain.
Which Dietary Adjustments Can Help Reduce Symptoms?
Adopting an anti-inflammatory diet that includes omega-3 rich foods and leafy greens while reducing processed foods and sugars can lower pro-inflammatory cytokines. Many patients report better digestive function and lower pain levels by making these dietary changes.
What Emerging Treatments and Research Are Shaping Endometriosis Care?

The future of endometriosis care is being redefined by groundbreaking research and innovative treatments. Scientists and clinicians are exploring new therapies that go beyond symptom control, aiming for earlier diagnosis, targeted treatment, and long-term relief. These emerging approaches are bringing fresh hope to patients and transforming how this complex condition is understood and managed.
What New Therapies Are Being Tested in Clinical Trials?
New therapies in clinical trials include selective progesterone receptor modulators, novel anti-inflammatory agents, and histone deacetylase inhibitors. These approaches aim to reduce lesion growth at the molecular level, with early studies showing promising reductions in pain and lesion size within 12 weeks.
How Are Personalized Treatment Approaches Improving Outcomes?
Personalized medicine uses genetic, hormonal, and environmental profiling to tailor treatments. Biomarkers and advanced imaging help clinicians select the best therapy, leading to improved adherence and symptom control while minimizing side effects.
What Are the Promising Non-Hormonal Treatments on the Horizon?
Research into non-hormonal options focuses on drugs that inhibit angiogenesis and modulate immune responses. Advances in nanotechnology may soon enable direct delivery of anti-inflammatory agents to lesions, potentially reducing systemic side effects.
How Can You Choose the Best Endometriosis Treatment for Your Needs?

Selecting the right treatment involves careful consideration of symptoms, disease severity, fertility goals, and overall health:
What Factors Should Influence Your Treatment Choice?
Key factors include symptom severity, the extent of deep infiltrating endometriosis, previous treatment responses, and personal health history. A comprehensive evaluation, often involving imaging and diagnostic laparoscopy, helps guide optimal therapy selection.
How Can a Treatment Comparison Table Help You Decide?
A comparison table can outline various treatments by efficacy, side effects, duration, and cost. This clear, visual format assists patients in weighing trade-offs and choosing the therapy that aligns best with their needs.
When Should You Consult a Specialist for Endometriosis Care?
If initial treatments fail or symptoms persist, consulting a specialist is crucial. Experts in endometriosis can provide personalized treatment plans and up-to-date advice, particularly if pain, menstrual difficulties, or fertility issues are present.
Where Can You Find Support and Resources for Endometriosis Treatment?

Managing endometriosis goes beyond medical treatment—it requires a strong support system and the right tools to navigate daily challenges. From connecting with others who share your experience to seeking expert medical guidance and using technology to track your symptoms, multiple resources are available to help you take control of your health. Here’s how to find the support and information you need on your endometriosis journey.
What Patient Support Groups Are Available?
Support groups, such as those organized by the Endometriosis Association, connect patients for sharing experiences, advice, and emotional support. These communities improve mental health and help patients feel less isolated.
How Can Expert Opinions Inform Your Treatment Plan?
Specialists—gynecologists, pain experts, and reproductive endocrinologists—offer essential insights into the latest treatments and emerging research. Their expertise ensures comprehensive care that addresses both physical and emotional aspects of the disease.
What Tools Can Help Track Symptoms and Treatment Effectiveness?
Digital tools like symptom journals, mobile apps, and wearable devices help patients monitor pain, menstrual cycles, and overall well-being. This data is valuable for adjusting treatments and enhancing adherence to therapy plans.
Frequently Asked Questions
Q: What are the primary goals of endometriosis treatment? A: The goals are to relieve pain, reduce lesion size, prevent disease progression, and improve fertility. Treatment plans are customized using hormonal, surgical, and lifestyle approaches.
Q: How long does it typically take for hormonal therapies to show results? A: Results can vary from a few weeks to several months. Birth control pills may provide relief within one to three months, while GnRH agonists might require longer treatment with careful monitoring.
Q: Are there non-surgical options for managing endometriosis symptoms? A: Yes. Hormonal therapies, NSAIDs, and complementary methods like acupuncture and diet modifications offer effective management for many women, particularly those with mild to moderate symptoms.
Q: What factors determine whether surgery is necessary? A: Surgery is considered if symptoms are severe, medical treatments fail, or the disease is extensive. Factors include lesion extent, patient response to therapy, and fertility goals.
Q: Can lifestyle changes make a difference in management? A: Absolutely. Regular exercise, anti-inflammatory diets, and stress reduction techniques can reduce symptoms by up to 40% and support overall treatment efficacy.
Q: What emerging treatments show promise? A: New therapies, including histone deacetylase inhibitors, angiogenesis inhibitors, and immunomodulatory drugs, are being tested for molecular-level management of endometriosis.
Q: How important is patient support? A: Extremely important. Support groups, counseling, and regular consultations with healthcare professionals significantly improve treatment adherence and quality of life.
Final Thoughts
Endometriosis treatment requires balancing medical, surgical, and lifestyle interventions to manage symptoms effectively. Understanding the variety of therapies—from hormonal treatments and pain management to minimally invasive surgeries and complementary options—allows patients to work closely with specialists for personalized care. Ongoing research and emerging treatments continue to offer hope for more effective, tailored strategies to improve the quality of life for women with endometriosis.

