Manual therapy is a complementary, noninvasive treatment option that can play an important role in managing endometriosis-related pain. Rather than targeting endometrial lesions directly, manual therapy focuses on the musculoskeletal and connective tissue components that often contribute to persistent pelvic discomfort. Chronic inflammation, surgical history, and prolonged muscle guarding can lead to tight pelvic floor muscles, restricted fascia, joint stiffness, and the development of painful trigger points. Skilled hands-on techniques aim to restore mobility, reduce tissue tension, improve circulation, and calm the nervous system’s pain response. This article explores how manual therapy works, outlines the most commonly used techniques, explains the potential benefits for pelvic pain and function, and describes what patients can expect during a consultation at the Endometriosis Center of Excellence.
Research further supports this view by showing how chronic pelvic pain in endometriosis can be complex and multi‑factorial.
Endometriosis Pain: Addressing Myofascial Dysfunction & Sensitization
Chronic pelvic pain is a frustrating symptom for patients with endometriosis and is frequently refractory to hormonal and surgical management. While these therapies target ectopic endometrial lesions, they do not directly address pain due to central sensitization of the nervous system and myofascial dysfunction, which can continue to generate pain from myofascial trigger points even after traditional treatments are optimized. This article provides a background for understanding how endometriosis facilitates remodeling of neural networks, contributing to sensitization and generation of myofascial trigger points. Treatments that specifically address myofascial pain secondary to spontaneously painful myofascial trigger points and their putative mechanisms of action are also reviewed, including physical therapy, dry needling, anesthetic injections, and botulinum toxin injections.
Relating chronic pelvic pain and endometriosis to signs of sensitization and myofascial pain and dysfunction, KJ Heyrana, 2017
What Is Manual Therapy and How Does It Help Endometriosis Pain?
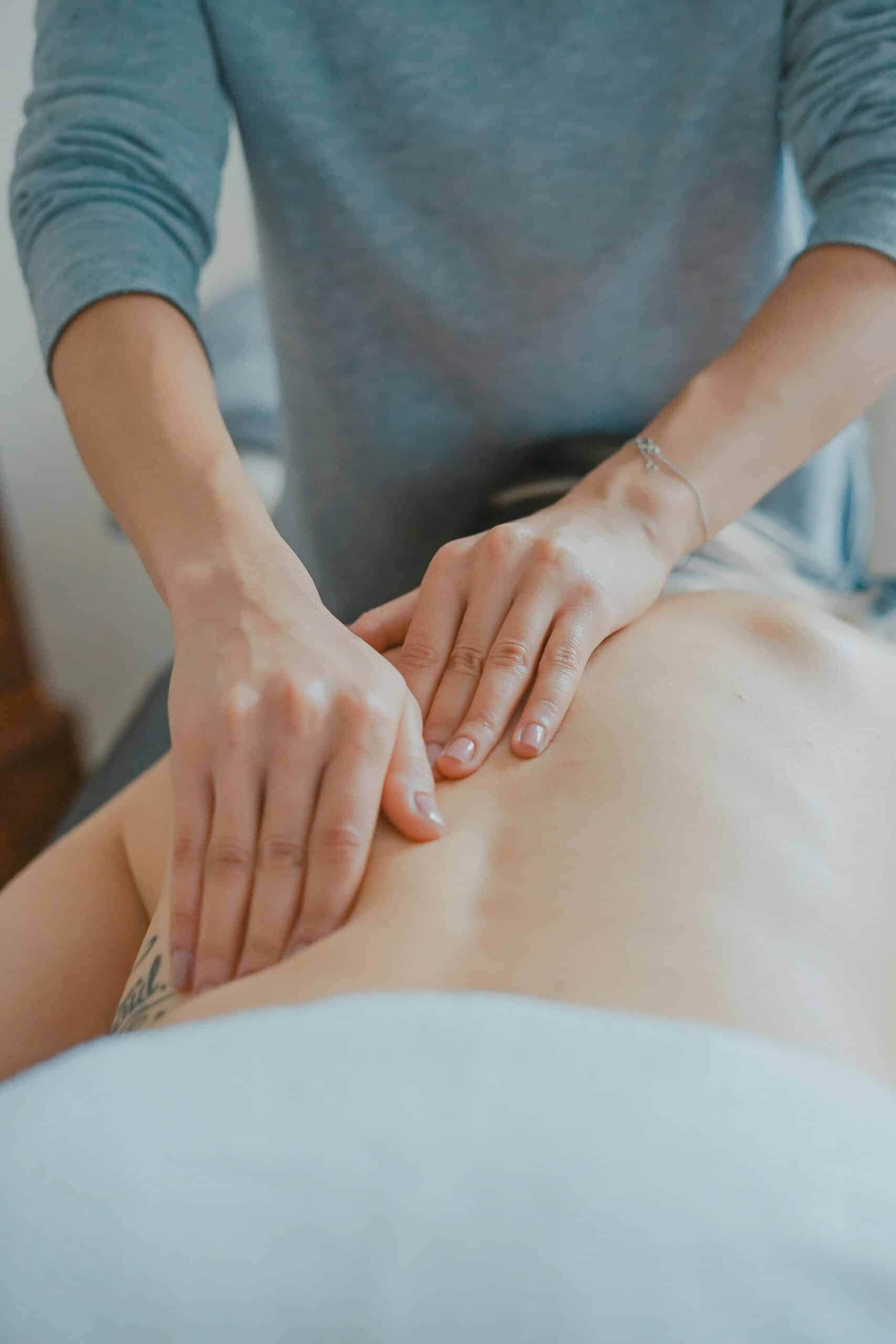
Manual therapy is a hands-on treatment approach designed to relieve pain, restore movement, and improve overall function. Trained therapists use targeted techniques to assess and treat soft tissues, joints, and connective structures that may be contributing to discomfort. By applying controlled pressure and specific mobilization methods, they work to reduce muscle tension, improve joint mechanics, enhance tissue flexibility, and stimulate healthy circulation. These changes can help calm the nervous system and interrupt chronic pain patterns that develop over time.
Understanding Manual Therapy and Pelvic Floor Therapy for Endometriosis
Techniques such as myofascial release and deep tissue massage target the pelvic floor to reduce tension, improve tissue mobility, and support lymphatic flow. Many patients report less pain after treatment, especially when manual therapy is part of a broader care plan.
How Manual Therapy Targets Pelvic Pain and Dysfunction
Therapists identify pelvic dysfunctions, then use targeted releases and mobilizations. Myofascial release eases fascia tension; deep tissue work addresses tight muscles. When combined with other care, regular sessions can improve alignment, mobility, and chronic pain.
Further research examines the physiological mechanisms by which manual therapy can reduce pain and improve mobility.
How Manual Therapy Reduces Endometriosis Pain & Improves Mobility
our site-specific manual therapy appears to deform or cause failure of adhesive crosslink bonds, which in turn decreases pain, and appears to improve visceral mobility.
Decreasing dyspareunia and dysmenorrhea in women with endometriosis via a manual physical therapy: results from two independent studies, 2011
Which Manual Therapy Techniques Are Used for Endometriosis Symptom Management?

Several manual therapy techniques can help manage endometriosis symptoms by addressing the musculoskeletal and connective tissue components of chronic pelvic pain. These techniques may include soft tissue mobilization, myofascial release, trigger point therapy, joint mobilization, and scar tissue work when prior surgeries are involved. Each approach is selected based on the individual’s pain presentation, pelvic floor muscle tone, mobility restrictions, and functional limitations. By reducing muscle overactivity, improving tissue glide, and restoring joint mechanics, manual therapy can decrease pain intensity and improve daily comfort.
Common Manual Therapy Methods for Pelvic Floor Dysfunction
The following manual therapy methods are frequently used to address pelvic floor dysfunction in women with endometriosis:
- Myofascial Release : Focuses on fascia tension to improve mobility.
- Deep Tissue Massage : Works deeper muscles to relieve chronic tightness.
- Lymphatic Drainage Massage : Gentle technique to support lymph flow and reduce swelling.
Used consistently, these methods can provide short‑term relief and support longer‑term pelvic health.
Benefits of Physical Therapy for Endometriosis Relief
Physical therapy can reduce pain, improve function, and enhance daily life when combined with other treatments.
- Reduction in Pain Levels : Regular sessions can reduce pelvic pain.
- Improved Quality of Life : Better mobility and less pain improve daily living.
- Complementary to Medical Treatments : Physical therapy can augment medical care.
These benefits support physical therapy as an important element in endometriosis care.
Who Is Eligible for Manual Therapy and What Is the Consultation Process?
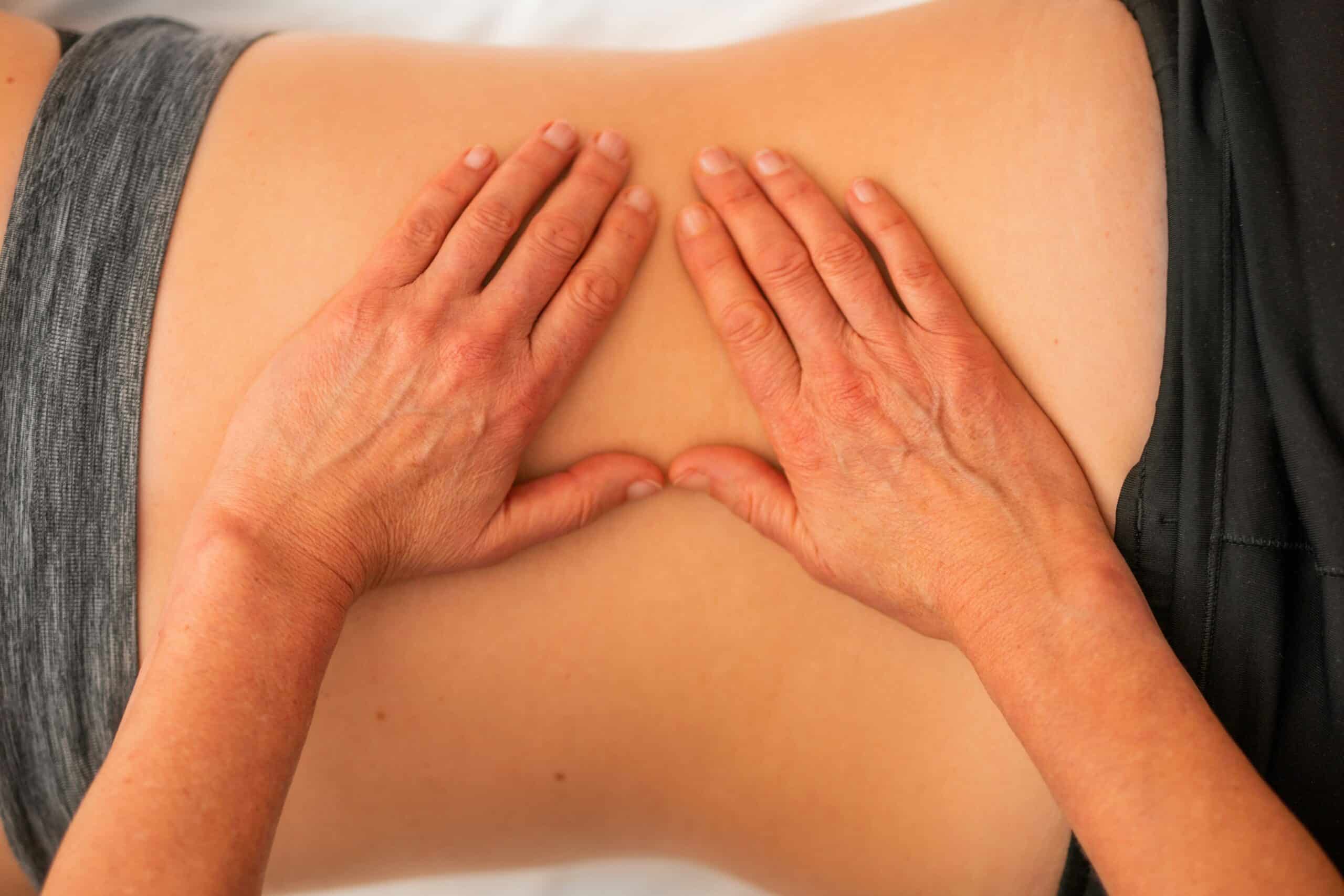
Understanding who is eligible for manual therapy and what the process involves can help you determine whether it is an appropriate part of your endometriosis treatment plan. Manual therapy is often recommended for individuals experiencing chronic pelvic pain, pelvic floor muscle tension, painful intercourse, post-surgical scar tightness, or persistent symptoms despite medical or hormonal treatment. It may also benefit those who notice increased pain with sitting, exercise, or bowel and bladder function. A thorough evaluation by a trained pelvic health specialist helps identify whether musculoskeletal factors are contributing to your symptoms and whether hands-on treatment could provide relief.
Patient Criteria for Manual Therapy at Endometriosis Center of Excellence
To qualify, patients usually need a confirmed diagnosis and symptoms suggesting pelvic pain or dysfunction. A medical history review ensures safety.
- Diagnosis of Endometriosis : A confirmed diagnosis is necessary.
- Presence of Pelvic Pain : Chronic pelvic pain may indicate benefit.
- Medical History Review : Review identifies contraindications and ensures suitability.
These checks help tailor treatment and keep care safe.
What to Expect During a Manual Therapy Consultation
Consultations include a full assessment to guide treatment choices at the Center.
- Initial Assessment Process : Evaluation of symptoms and history to shape the plan.
- Discussion of Treatment Goals : Patients set goals and expectations.
- Integration with Other Therapies : The plan will coordinate manual therapy with other care.
This assessment creates a personalised plan aligned with each patient’s goals.
How Manual Therapy Fits Into a Multidisciplinary Endometriosis Treatment Plan

Effective endometriosis management often requires more than a single intervention. Because the condition affects inflammatory pathways, pelvic floor muscles, connective tissues, and the nervous system, a multidisciplinary treatment plan provides more comprehensive and lasting relief. Manual therapy plays an important role within this integrated model by addressing the musculoskeletal and neuromuscular contributors to chronic pelvic pain. When coordinated with medical and supportive therapies, it helps create a more complete and individualized care strategy.
Integrating Manual Therapy With Gynecologic and Hormonal Care
Manual therapy is most effective when it is coordinated with gynecologic treatment, hormonal management, and, when necessary, surgical care. While medical therapies focus on suppressing or removing endometrial lesions, manual therapy addresses secondary musculoskeletal dysfunction such as pelvic floor muscle overactivity, scar tissue restriction, and joint stiffness. By combining these approaches, patients receive more comprehensive relief that targets both inflammation and the persistent pain patterns maintained by muscle guarding and nervous system sensitization.
Addressing Central Sensitization and Chronic Pain Patterns
Chronic pelvic pain in endometriosis is often multifactorial and may involve central sensitization, a condition in which the nervous system becomes hypersensitive to pain signals. Even after lesions are treated, the brain and spinal cord may continue amplifying discomfort. Manual therapy, particularly when paired with pelvic floor rehabilitation and pain neuroscience education, can help modulate this heightened pain response. Targeted hands-on techniques may reduce trigger point activity, improve tissue mobility, and provide therapeutic input that supports nervous system regulation over time.
Supporting Long-Term Function, Mobility, and Quality of Life
Beyond short-term pain relief, incorporating manual therapy into a broader care plan can improve long-term functional outcomes. Restoring pelvic mobility, improving alignment, and reducing muscle tension allows patients to sit, exercise, and engage in daily activities with greater comfort. When coordinated with physical therapy exercises, stress management strategies, and medical oversight, manual therapy supports sustainable improvements in mobility and overall quality of life. This integrated approach reflects current research emphasizing that effective endometriosis care must address inflammatory, neuromuscular, and psychosocial contributors to chronic pelvic pain.
What Evidence Supports Manual Therapy as a Non-Surgical Treatment for Endometriosis?

Recent studies and clinical reports suggest that manual therapy may help reduce pain and improve physical function in individuals with endometriosis, particularly when pelvic floor dysfunction and myofascial restrictions are present. Research examining chronic pelvic pain populations has shown that hands-on techniques such as myofascial release, trigger point therapy, and soft tissue mobilization can decrease muscle overactivity, improve tissue mobility, and reduce pain sensitivity. These improvements may translate into better tolerance for daily activities, decreased pain with intercourse, and improved bladder or bowel function when musculoskeletal factors contribute to symptoms.
Recent Clinical Studies on Manual Therapy Effectiveness
Clinical research reports reduced pain after treatment series in some studies. These findings support manual therapy as part of multi-modal care.
Indeed, a recent randomized clinical trial reinforces the potential value of manual therapy as a complementary treatment.
Manual Therapy: A Complementary Approach for Endometriosis Pain Relief
In conclusion, manual therapy may be an excellent complement to the gynecological treatment of endometriosis-related pelvic pain by alleviating pain and improving women’s endometriosis-related quality of life.
Effectiveness of a manual therapy protocol in women with pelvic pain due to endometriosis: a randomized clinical trial, 2023
Patient Testimonials and Success Stories with Manual Therapy
Many patients report less pain, improved mobility, and greater well‑being. Testimonials provide practical insight into treatment effects.
Frequently Asked Questions
What are the potential side effects of manual therapy for endometriosis?
Manual therapy is generally safe; temporary soreness, bruising, or fatigue can occur. These effects usually resolve quickly. Report discomfort so your therapist can adapt techniques. A medical review helps identify rare risks.
How often should I undergo manual therapy for optimal results?
Frequency depends on symptoms and goals. Many start weekly for a few weeks, then move to less frequent maintenance sessions as progress is made.
Can manual therapy be combined with other treatments for endometriosis?
Yes. Manual therapy complements medications, hormonal care, and surgery. Coordinate with your healthcare team to align treatments.
Is manual therapy suitable for all women with endometriosis?
It can help many, but not everyone. Disease severity, comorbidities, and contraindications affect suitability. An assessment determines fit and safety.
What qualifications should a therapist have to provide manual therapy for endometriosis?
Choose licensed physical/manual therapists with pelvic health training. Certifications or experience in pelvic floor therapy improve outcomes.
How long does it typically take to see results from manual therapy?
Results vary. Some see change in a few sessions; others need weeks of consistent treatment. Severity, individual response, and adherence affect timing.
Conclusion
Manual therapy is a non‑invasive option to reduce endometriosis-related pain, improve mobility, and enhance quality of life. It addresses pelvic dysfunction and can complement standard medical care. Discuss manual therapy with your care team to see if it fits your plan.

