Endometriosis commonly causes pelvic pain and disrupts daily life. Manual therapy specialized for endometriosis includes hands-on, non-surgical treatments that can reduce symptoms and improve quality of life. This article summarizes common manual techniques, how pelvic floor physical therapy helps, and how these therapies fit into broader pain-management plans, with patient perspectives. Understanding the role of manual therapy in managing endometriosis is crucial for patients seeking alternatives or complements to medical and surgical treatments. These therapies focus on addressing musculoskeletal and fascial components of pain, which are often overlooked in conventional care.
Emerging research and clinical experience show non‑medical approaches like manual therapy can meaningfully improve quality of life. These approaches emphasize a holistic view of health, recognizing the interconnectedness of physical, emotional, and psychological factors in chronic pain conditions such as endometriosis. By integrating manual therapy into comprehensive care plans, patients may experience enhanced symptom relief and improved overall well-being.
Which Manual Therapy Techniques Can Ease Pelvic Pain from Endometriosis?
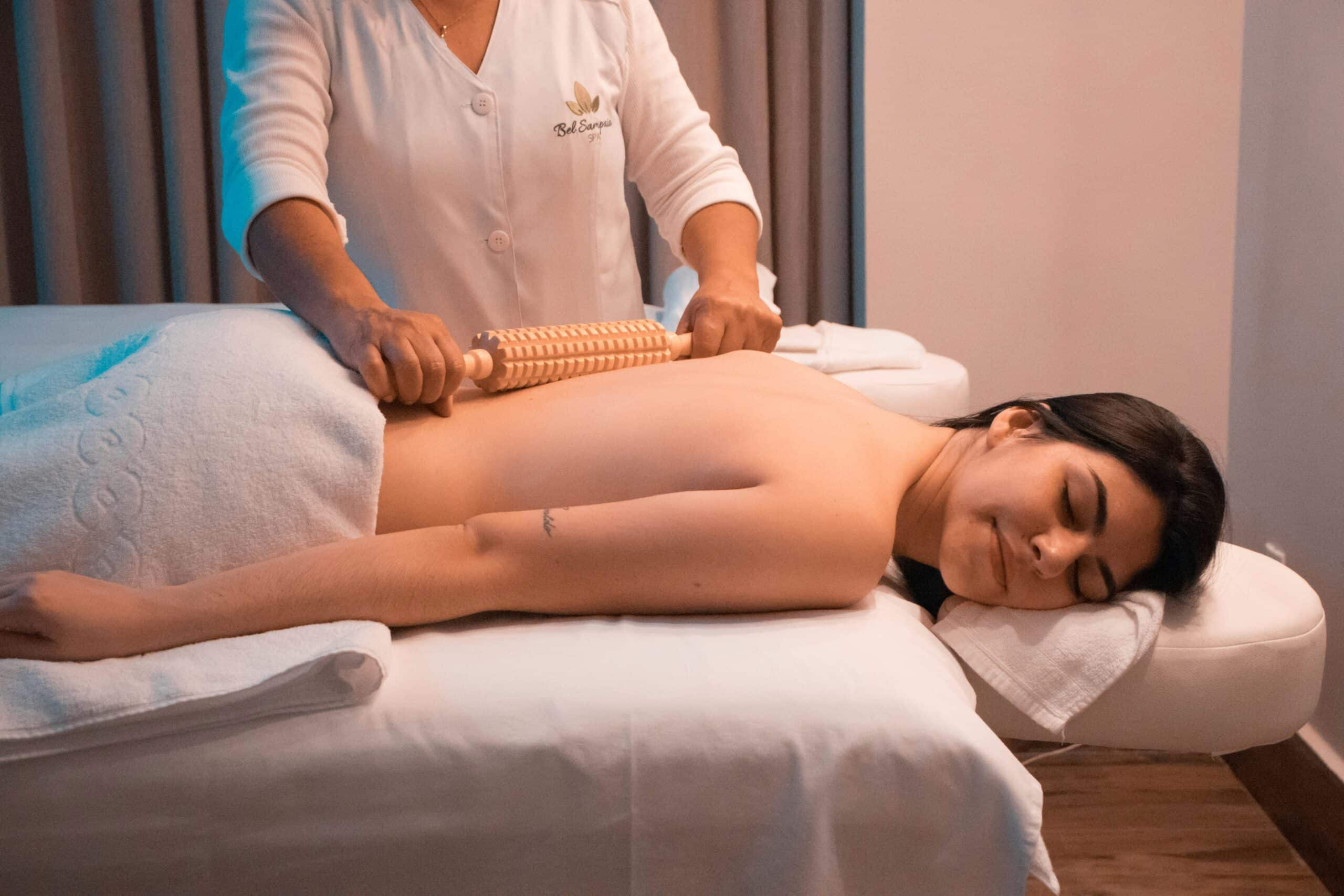
Manual therapy includes Swedish and deep tissue massage, myofascial release, and targeted soft‑tissue work to reduce tension, relax muscles, and improve local blood flow. These techniques are designed to address the musculoskeletal components of pelvic pain, which can be exacerbated by endometriosis-related inflammation and adhesions. By improving circulation and reducing muscle tightness, manual therapy can help alleviate pain and improve mobility in the pelvic region.
Therapists often tailor these techniques to the individual’s specific symptoms and areas of discomfort, ensuring a personalized approach that maximizes benefits. The hands-on nature of manual therapy also allows practitioners to identify and address subtle restrictions or trigger points that may contribute to persistent pain.
How Does Pelvic Floor Physical Therapy Help Endometriosis Symptoms?
Pelvic floor physical therapy targets the muscles and connective tissues that support pelvic organs. Improving mobility, easing muscle tension, and retraining coordination can reduce pain and restore function. Guided sessions and home exercises help when tightness contributes to discomfort. pelvic floor therapy This specialized therapy addresses dysfunctions such as muscle spasms, trigger points, and poor muscle coordination that often accompany endometriosis. By restoring normal muscle function, pelvic floor physical therapy can reduce pain during activities such as sitting, walking, and sexual intercourse.
Studies show PT benefits a wide range of patients, including adolescents and young adults. Early intervention with pelvic floor therapy may prevent chronic pain development and improve long-term outcomes. Therapists also provide education on posture, body mechanics, and self-care strategies to empower patients in managing their symptoms independently.
What Role Does Myofascial Release Play in Managing Endometriosis Pain?
Myofascial release works on fascia the connective tissue around muscles to reduce restrictions that can cause persistent pelvic pain. Targeted release may improve movement and daily function. Fascia can become tight or adhered due to inflammation or surgical scarring, contributing to pain and limited mobility. Myofascial release techniques aim to gently stretch and loosen these tissues, promoting better elasticity and circulation.
Clinical practice increasingly links myofascial dysfunction to chronic pelvic pain, so targeted physical therapy is often part of comprehensive care. Addressing myofascial restrictions can also reduce nerve irritation and improve the overall function of the pelvic region. Patients often report a sense of relief and increased comfort following these treatments.
What Are the Key Benefits of Physical Therapy for Endometriosis Patients?
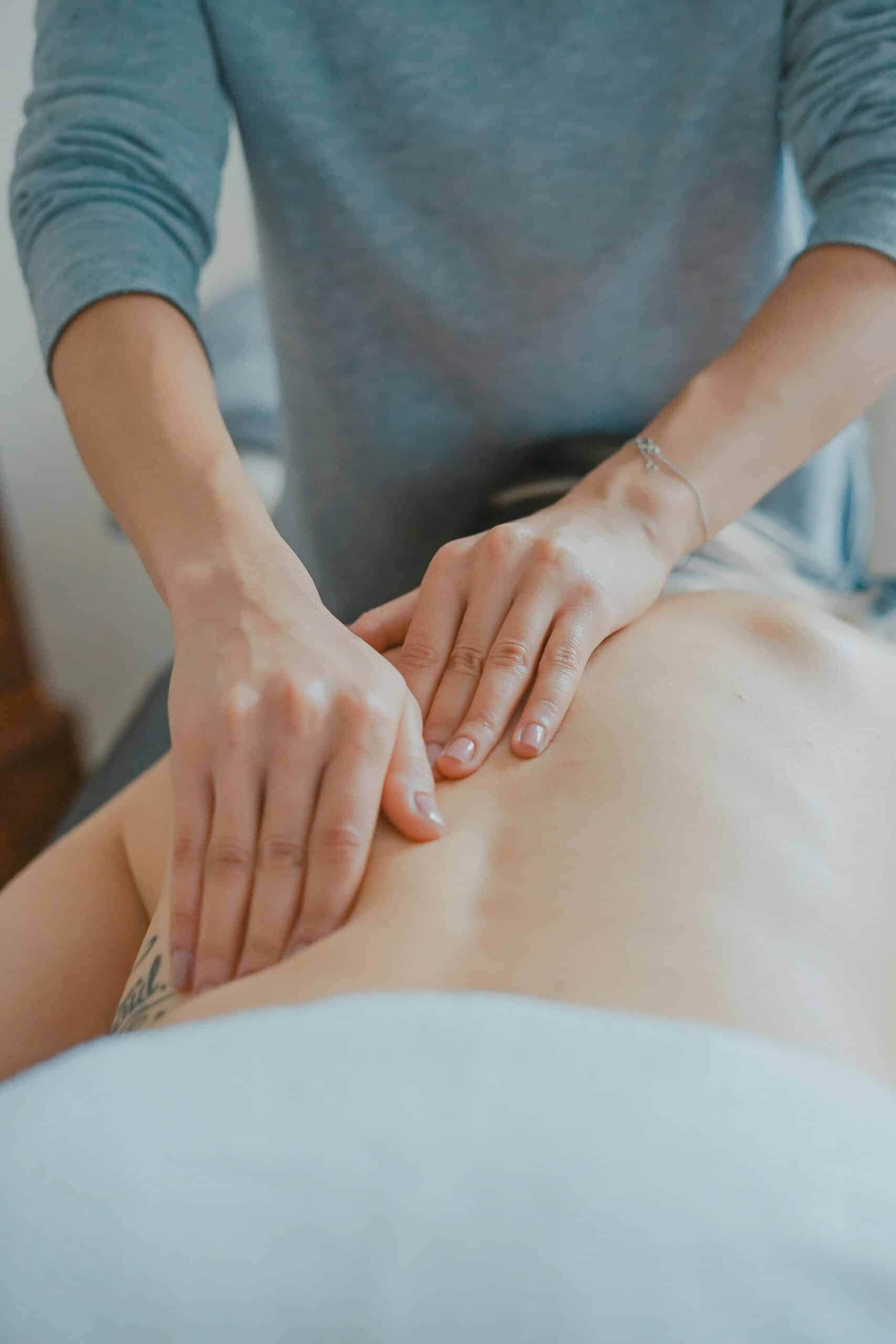
Physical therapy can reduce pain, improve pelvic mobility and muscle function, and help people carry out daily activities. Benefits stem from manual techniques, therapeutic exercise, and education tailored to individual needs. By addressing both the physical and functional aspects of pelvic pain, physical therapy supports patients in regaining control over their bodies and improving their quality of life.
Therapists often work closely with patients to develop personalized treatment plans that incorporate lifestyle modifications and self-management strategies. This comprehensive approach helps sustain improvements and prevent symptom recurrence.
How Does Manual Therapy Reduce Pelvic Pain and Improve Muscle Function?
Manual therapy releases tight muscles, improves tissue flexibility, and restores movement patterns. Many patients report less pain and better function after treatments such as deep tissue massage and myofascial work. These techniques can also help break down adhesions and scar tissue that may contribute to restricted movement and discomfort.
Regular sessions combined with home exercises can enhance muscle strength and coordination, further supporting pain reduction and functional gains. The hands-on nature of manual therapy also provides immediate feedback and adjustment, allowing therapists to respond to patient needs dynamically.
Can Manual Lymphatic Drainage Enhance Symptom Relief in Endometriosis?
Manual lymphatic drainage uses gentle, rhythmic strokes to encourage lymph flow and may reduce local swelling or congestion, easing pelvic discomfort for some patients. This technique supports the body’s natural detoxification processes and can help alleviate inflammation associated with endometriosis.
While evidence is still emerging, some patients report improvements in pelvic heaviness and bloating following lymphatic drainage sessions. It is often used as part of a multimodal approach to symptom management, complementing other manual and physical therapies.
How Can Non‑Surgical Treatments Complement Endometriosis Pain Management?

Non‑surgical options work best combined with medications, lifestyle changes, and mind‑body strategies to create a personalized plan that manages pain and improves function. Integrating these approaches allows for a more comprehensive management of endometriosis, addressing not only physical symptoms but also emotional and psychological well-being.
Collaborative care involving gynecologists, physical therapists, nutritionists, and mental health professionals can optimize outcomes and support patients throughout their treatment journey.
What Lifestyle Modifications Support Manual Therapy Outcomes?
Small, sustainable changes support manual therapy. Useful adjustments include:
- Dietary Adjustments : Emphasize anti‑inflammatory foods such as vegetables, fruits, whole grains, and omega‑3 sources. These foods may help reduce systemic inflammation and support overall health, potentially easing endometriosis symptoms.
- Regular Exercise : Gentle, low‑impact activities like walking, yoga, or swimming support circulation and pelvic health. Exercise also promotes endorphin release, which can improve mood and pain tolerance.
- Stress Management Techniques : Mindfulness, breathing work, and paced relaxation reduce tension and improve coping. Managing stress is important as it can exacerbate pain perception and muscle tightness.
Combined with therapy, these changes strengthen results and support long‑term well‑being. Patients are encouraged to adopt habits that promote resilience and self-care, enhancing the effectiveness of manual and physical therapies.
When Should Patients Consider Manual Therapy as Part of Their Treatment Plan?
Consider manual therapy when pelvic pain persists and affects daily life, intimacy, or mental health. Discuss options with your healthcare team so treatment fits your health, past care, and goals. Early referral to manual therapy can prevent chronic pain cycles and improve functional outcomes.
Patients experiencing symptoms such as pelvic muscle tightness, pain during intercourse, or difficulty with bowel or bladder function may particularly benefit from evaluation by a pelvic health specialist. Collaborative decision-making ensures that manual therapy is integrated appropriately within a broader treatment strategy.
How Do Patient Experiences Reflect the Effectiveness of Manual Therapy for Endometriosis?

Patient reports often describe meaningful pain reduction, improved movement, and better quality of life after targeted physical therapy and hands‑on care. These testimonials highlight the value of individualized treatment plans and the importance of addressing musculoskeletal contributors to pelvic pain.
Many patients emphasize the empowerment gained through education and self-management techniques learned during therapy, which help maintain improvements and reduce reliance on medications.
What Success Stories Highlight Improvements from Pelvic Floor Therapy?
Many describe regained function: returning to work, exercise, or daily activities after pelvic floor therapy. Individualized plans and consistent follow‑up are common themes in progress. Patients often report enhanced confidence in managing their symptoms and improved emotional well-being as a result of reduced pain and increased physical capacity.
Success stories also underscore the importance of a supportive therapeutic relationship and ongoing communication between patients and providers to adapt treatment as needed.
How Do Testimonials Support the Use of Manual Therapy in Endometriosis Care?
Testimonials show that hands‑on care can improve pain control and daily comfort, adding practical support for multidisciplinary, conservative care. Patients frequently note improvements in sleep quality, mood, and social participation, which contribute to overall quality of life.
These personal accounts reinforce clinical findings and encourage wider adoption of manual therapy as a valuable component of endometriosis management.
Frequently Asked Questions
What is the role of diet in managing endometriosis symptoms alongside manual therapy?
Diet supports symptoms: an anti‑inflammatory diet rich in vegetables, fruits, whole grains, and omega‑3s may help. Limiting processed foods and added sugars can also assist; diet complements therapy but does not cure endometriosis. Nutritional support can reduce systemic inflammation and improve energy levels, which may enhance the effectiveness of manual therapy and overall symptom management.
How often should patients undergo manual therapy for optimal results?
Frequency varies. Many start weekly for acute issues, then reduce to every two weeks or monthly for maintenance. Your therapist will tailor the schedule. Consistency is important to achieve lasting benefits, and adjustments are made based on symptom changes and treatment response.
Are there any risks or side effects associated with manual therapy for endometriosis?
Manual therapy is low risk with trained pelvic health professionals. Temporary soreness or fatigue can occur. Share your pain levels and medical history so techniques are adapted; some conditions may make specific techniques inappropriate. Open communication with your therapist ensures safe and effective care tailored to your needs.
Can manual therapy be combined with other treatments for endometriosis?
Yes. Manual therapy commonly complements medications, hormonal treatments, acupuncture, and lifestyle strategies. Coordinate care with your providers to ensure treatments are complementary. Integrating multiple approaches can address different aspects of endometriosis and improve overall outcomes.
What should patients expect during their first manual therapy session?
Expect a detailed history and assessment of posture, movement, and pelvic function. The therapist will discuss goals and may start gentle hands‑on work or prescribe exercises. Some short‑lived discomfort can occur; painful procedures should be avoided or modified. The initial session also includes education about the condition and treatment plan to set realistic expectations.
How can patients find qualified manual therapists for endometriosis treatment?
Look for clinicians specializing in pelvic or women’s health physical therapy. Ask for referrals, check directories, review therapist profiles for training and endometriosis experience, and schedule a brief consultation to assess fit. Ensuring the therapist has specific expertise in pelvic pain and endometriosis is important for effective care.
Conclusion
Manual therapy can be a useful non‑surgical option for people with endometriosis, offering pain relief and improved pelvic function. Paired with a personalized plan and lifestyle changes, hands‑on therapies can help reclaim function and quality of life. Talk with your care team to choose an approach that matches your goals and needs. As research continues to evolve, manual therapy remains a promising adjunct to traditional treatments, empowering patients to take an active role in managing their condition and enhancing their overall well-being.

