Endometriosis is a long-term condition that can cause significant pelvic pain and disrupt daily life. Pelvic floor physical therapy is increasingly recognized as a key part of care: it uses focused, hands‑on and exercise-based strategies to ease symptoms and restore function. This article explains how physical therapy helps people with endometriosis, reviews the role of pelvic floor dysfunction, outlines effective treatment techniques, and describes the benefits patients commonly experience. We also explain how to find specialized pelvic floor physical therapy services.
What Is Pelvic Floor Dysfunction in Endometriosis and How Does It Affect Recovery?

Pelvic floor dysfunction describes problems with the muscles and connective tissues that support the pelvic organs. When endometriosis is present, inflammation and pain can lead to increased muscle tension, spasms, and poor coordination of the pelvic floor. These changes contribute to chronic pelvic pain, urinary symptoms, and sexual pain, and they can slow recovery by limiting movement and increasing sensitivity. Recognizing how endometriosis and pelvic floor dysfunction interact helps clinicians design treatments that address both the physical and emotional sides of healing.
Studies have demonstrated a clear association between endometriosis and pelvic floor issues such as muscle spasm.
Pelvic Floor Muscle Spasms in Deep Endometriosis
In a study of 104 patients, researchers compared 52 people with deep endometriosis (G1) to 52 controls without endometriosis (G2). Each participant received a full physical therapy evaluation, including medical history, assessment for dyspareunia, and a detailed pelvic floor exam looking for muscle spasms, trigger points, and muscle function. The group with deep endometriosis showed a substantially higher prevalence of muscle spasms: 53.9% in G1 versus 17.3% in G2 (p < 0.001). The authors concluded that deep endometriosis is associated with increased pelvic floor muscle spasm compared with controls.
Assessment of pelvic floor muscles in women with deep endometriosis, 2016
How Endometriosis Contributes to Pelvic Floor Muscle Spasm and Chronic Pain
Endometriosis creates a cycle of inflammation and nerve sensitization within the pelvis. As pain signals continue, the nervous system may become hypersensitive, causing the pelvic floor muscles to contract involuntarily. This chronic tightening can lead to muscle spasms, trigger points, and reduced blood flow, all of which contribute to ongoing pelvic pain. Many patients experience symptoms such as painful intercourse, urinary urgency, constipation, or low back discomfort that stem from pelvic floor dysfunction rather than endometrial lesions alone. Research has demonstrated a strong association between endometriosis and pelvic floor muscle spasm, highlighting the importance of evaluating musculoskeletal contributors when symptoms persist.
How Pelvic Floor Dysfunction Can Delay Recovery From Endometriosis
When pelvic floor dysfunction is present, recovery from endometriosis treatment can be slower and more complex. Even after surgery or hormonal therapy reduces active lesions, tight or poorly coordinated pelvic muscles may continue to generate pain. Limited movement, muscle stiffness, and heightened pain sensitivity can also affect emotional well-being and overall quality of life. Addressing both endometriosis and pelvic floor dysfunction through a comprehensive treatment plan, including pelvic floor physical therapy, improves outcomes by targeting the mechanical, neurological, and functional aspects of pain. This integrated approach supports more complete healing and long-term symptom management.
Which Physical Therapy Techniques Are Effective for Endometriosis Recovery?
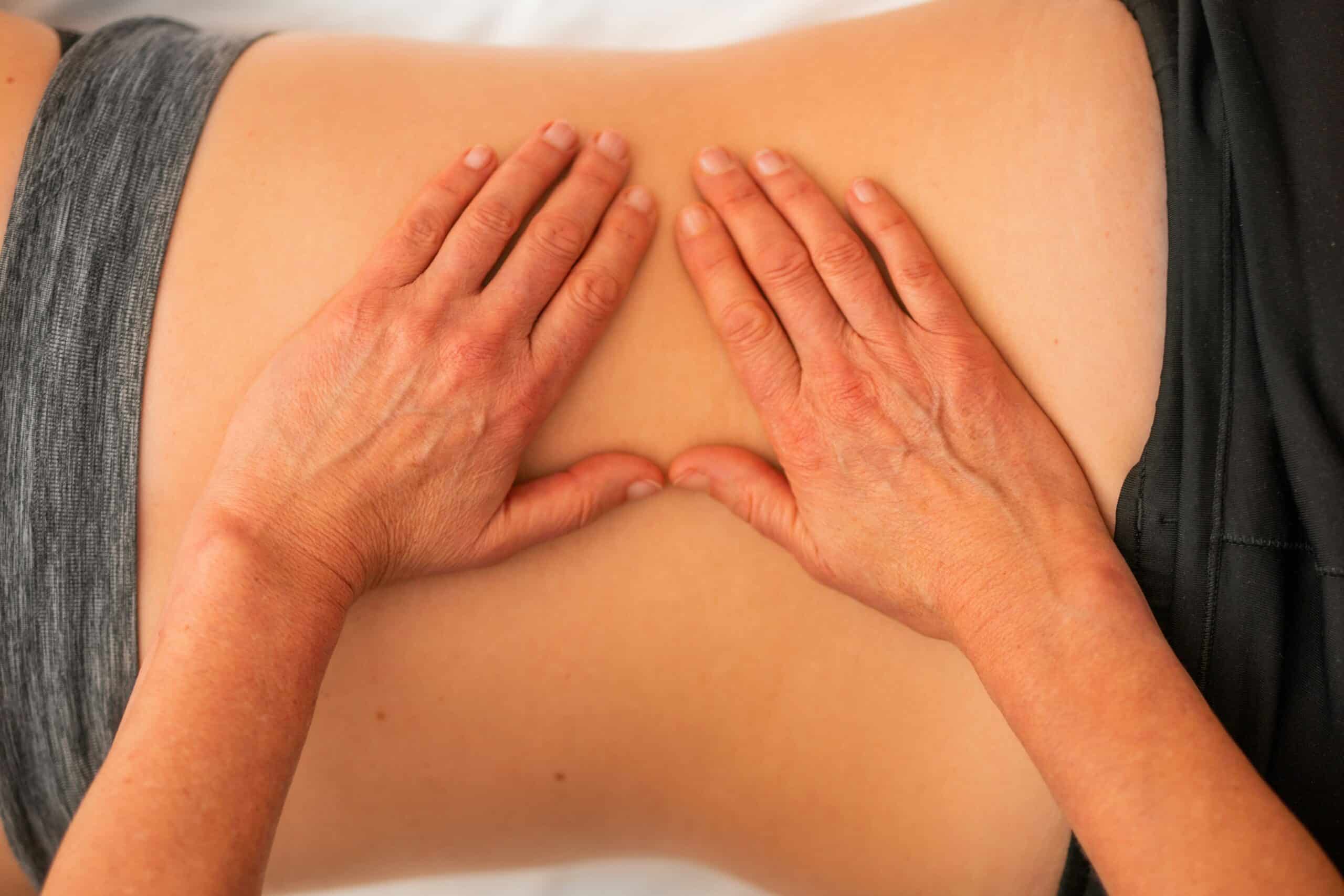
Multiple physical therapy approaches can help manage endometriosis-related symptoms by addressing the musculoskeletal and neuromuscular components of chronic pelvic pain. While endometriosis is driven by inflammatory and hormonal factors, persistent pain often involves secondary pelvic floor dysfunction, muscle guarding, and connective tissue restrictions. Evidence-informed pelvic floor physical therapy techniques focus on restoring normal movement patterns, reducing protective muscle tension, and improving overall pelvic function.
- Manual Therapy : Skilled, hands-on techniques to ease pelvic floor muscle tension, restore joint and soft-tissue mobility, and reduce pain.
- Myofascial Release : Targeted work on the fascia surrounding pelvic muscles to break up tightness, improve tissue glide, and support normal movement.
- Trigger Point Therapy : Direct treatment of localized tender spots to decrease referred pain and improve overall pelvic function.
These therapeutic approaches are effective because they address myofascial dysfunction and persistent trigger points that continue to generate symptoms even after hormonal therapy or surgical treatment. By treating the mechanical and neuromuscular contributors to pain, pelvic floor physical therapy provides a complementary strategy that supports long-term symptom management and improved quality of life.
Endometriosis Pain: Understanding Myofascial Dysfunction & Physical Therapy
Chronic pelvic pain in endometriosis can persist despite hormonal or surgical care because of central nervous system sensitization and myofascial pain. These processes may create painful myofascial trigger points that keep generating pain after lesion-directed treatments are optimized. The article outlines how endometriosis can remodel neural networks and contribute to sensitization, offers a clinical framework for evaluating myofascial trigger points and sensitization, and reviews interventions that address myofascial pain—such as physical therapy, dry needling, anesthetic injections, and botulinum toxin—along with their proposed mechanisms.
Relating chronic pelvic pain and endometriosis to signs of sensitization and myofascial pain and dysfunction, KJ Heyrana, 2017
People seeking specialized care often find pelvic floor physical therapists with training in women’s health who build individualized programs combining these techniques, exercise, education, and pain‑management strategies to support recovery.
Manual Therapy
Manual therapy involves skilled, hands-on techniques performed by a trained pelvic health physical therapist. These techniques may include gentle internal and external soft tissue mobilization, joint mobilization of the hips and sacroiliac joints, and stretching of shortened pelvic floor muscles. The goal is to reduce muscle overactivity, improve circulation, and restore normal mobility in the surrounding structures. For individuals with endometriosis, chronic pain can cause the pelvic floor muscles to remain in a guarded state, which perpetuates discomfort even between flare-ups. Manual therapy helps interrupt this cycle by decreasing tension and improving tissue flexibility.
Myofascial Release
Myofascial release targets the fascia, which is the connective tissue that surrounds and supports muscles and organs. In endometriosis, inflammation, past surgeries, and chronic muscle tightening can lead to fascial restrictions that limit movement and contribute to pain. Through sustained, gentle pressure applied to specific areas, a therapist works to release tight or adhered tissue and improve tissue glide. Improving fascial mobility can reduce pulling sensations, enhance pelvic alignment, and support more normal muscle function. Over time, this can decrease pain during activities such as sitting, exercise, or intercourse.
Trigger Point Therapy
Trigger point therapy focuses on treating localized areas of muscle that are hyperirritable and tender to the touch. These trigger points can refer pain to other areas of the pelvis, lower abdomen, hips, or low back, making symptoms feel widespread or difficult to pinpoint. A pelvic floor physical therapist may use sustained pressure, dry needling when appropriate, or other techniques to deactivate these painful spots. Reducing trigger point activity can decrease referred pain patterns, improve muscle coordination, and enhance overall pelvic stability.
What Are the Benefits and Expected Outcomes of Physical Therapy for Endometriosis?

Pelvic floor physical therapy can deliver meaningful benefits for people with endometriosis. Common outcomes include:
- Pain relief : Targeted therapy can reduce chronic pelvic pain and make daily activities more manageable.
- Improved quality of life : Addressing physical dysfunction and coping strategies often leads to better sleep, mood, and overall function.
- Potential fertility support : By reducing pelvic tension and improving circulation, some interventions may create a more favorable reproductive environment; however, current evidence is limited and more research is needed.
A growing body of research supports the wide-ranging rehabilitation benefits for people with endometriosis.
Physical Therapy for Endometriosis: A Systematic Review of Rehabilitation Benefits
Objectives: This review aimed to summarize recent evidence on the effectiveness of rehabilitation interventions for symptoms related to endometriosis and adenomyosis. Methods: The review protocol was registered (CRD42022236516). Researchers searched Medline, Web of Science, and Scopus for studies published through 23 July 2025 that evaluated rehabilitation interventions in women with endometriosis or adenomyosis. Risk of bias was assessed and meta-analyses were performed. Results: From 970 identified records, 19 reports from 17 trials met inclusion criteria. About one-third of trials investigated electrophysical agents, another third evaluated exercise programs, and the remaining studies included manual therapy–based interventions such as pelvic floor physiotherapy or Swedish massage alongside other modalities. Most trials measured changes in pain and quality of life (QoL).
Impact of Physical Rehabilitation on Endometriosis and Adenomyosis-Related Symptoms: A Systematic Review and Meta-Analysis, 2025
The table below summarizes common techniques, what they address, and the outcomes patients typically experience:
These findings emphasize the value of including physical therapy in a comprehensive, multidisciplinary treatment plan for endometriosis.
How Can Patients Access Specialized Pelvic Floor Physical Therapy for Endometriosis?

To find specialized pelvic floor physical therapy, start by asking your healthcare provider for a referral to a pelvic health clinician or searching for therapists credentialed in women’s pelvic health. Clinics that focus on pelvic pain or Endometriosis Centers of Excellence often provide multidisciplinary care that coordinates physical therapy with gynecology, pain management, and behavioral health. Local professional directories and national pelvic health associations are also useful resources for locating qualified providers.
Get a Referral to a Pelvic Health Specialist
Start by speaking with your gynecologist, primary care provider, or endometriosis specialist about pelvic floor physical therapy. Many providers maintain referral networks that include clinicians trained specifically in pelvic health. A direct referral not only streamlines the process but also ensures coordinated care between your medical team and physical therapist. This collaboration is especially important for endometriosis-related pelvic pain, where treatment outcomes improve when providers communicate about symptoms, flare patterns, and surgical history.
Search for Therapists Credentialed in Women’s Pelvic Health
Not all physical therapists are trained in internal pelvic floor evaluation or chronic pelvic pain management. When researching providers, look for clinicians who specialize in women’s pelvic health and have advanced training in treating conditions like endometriosis, dyspareunia, and myofascial pelvic pain. Professional directories from national pelvic health associations can help you filter by specialty and credentials. Reviewing a clinic’s website for experience with endometriosis-specific care can also help confirm that the provider understands the complexity of this condition.
Consider Multidisciplinary Clinics or Endometriosis Centers
Clinics that focus on pelvic pain or are recognized as Endometriosis Centers of Excellence often offer integrated care models. These centers may coordinate pelvic floor physical therapy with gynecology, pain management, and behavioral health support. Because endometriosis affects multiple systems including musculoskeletal, neurological, and hormonal systems, a multidisciplinary approach helps address both the physical and functional components of pain. Choosing a center with collaborative care can lead to more comprehensive symptom management and long-term improvement.
Frequently Asked Questions
What role does emotional support play in physical therapy for endometriosis?
Emotional support is a key part of recovery. Chronic pelvic pain can cause anxiety, frustration, and depression, which in turn affect pain and function. Physical therapists frequently use education, pacing, and coping strategies, and they often work alongside psychologists or counselors to address emotional health. A combined physical and emotional approach tends to improve long‑term outcomes.
Are there any risks associated with physical therapy for endometriosis?
Physical therapy is generally safe, but some people may feel temporary soreness or increased discomfort, especially if symptoms are severe. Careful assessment and an individualized plan reduce risk. Communicate openly with your therapist about pain levels and any concerns, and seek a clinician with experience treating endometriosis when possible.
How long does it typically take to see results from physical therapy?
Response time varies. Some people notice improvement after a few sessions; others need weeks to months of consistent therapy and home practice. Progress depends on symptom severity, coexisting conditions, and adherence to the program. Regular follow-up helps tailor the plan and track improvements.
Can physical therapy help with fertility issues related to endometriosis?
Physical therapy may support fertility indirectly by reducing pelvic tension, improving circulation, and normalizing pelvic mechanics factors that can create a healthier environment for conception. Evidence is promising but not definitive; patients with fertility concerns should discuss integrated reproductive care with their gynecologist and pelvic health team.
What should patients expect during their first physical therapy session?
Expect a thorough evaluation: a medical history review, conversation about symptoms and goals, and a pelvic floor assessment when appropriate and consented to. The clinician will explain findings and recommend a personalized plan that may include manual therapy, exercises, and self‑management strategies. Clear communication about comfort and boundaries is encouraged.
How can patients maintain progress after completing physical therapy?
To sustain gains, continue prescribed home exercises, stay active, practice pelvic health strategies, and use pain‑management tools you learned in therapy. Periodic check-ins with your therapist can help address new issues early. Joining support groups and staying informed about endometriosis can also help with long‑term self‑management.
Conclusion
Incorporating pelvic floor physical therapy into endometriosis care can provide meaningful pain relief, improve daily function, and support overall well‑being. By addressing both the body and the emotional effects of chronic pelvic pain, a tailored therapy plan can be an important step toward better health. If you’re ready to explore this option, our pelvic health specialists can help design a program that fits your needs.

