Endometriosis is a chronic and often debilitating condition characterized by persistent pelvic pain that significantly impacts daily life. While various treatments exist, physical therapy stands out as an evidence-informed approach to effectively ease symptoms and restore function. This comprehensive article explores how specialized interventions like pelvic floor rehabilitation, hands-on manual techniques, and tailored exercise programs can reduce pain and enhance quality of life. We’ll also delve into how physical therapy integrates with surgical preparation and recovery, empowering you to make informed treatment decisions. Supported by systematic reviews and clinical summaries, physiotherapy is recognized for its efficacy in reducing endometriosis pain symptoms and improving pelvic function.
What Is Pelvic Floor Physical Therapy and How Can It Help with Endometriosis?
Pelvic floor physical therapy assesses and treats pelvic muscles, connective tissue, and movement patterns to reduce pain, restore coordination, and improve pelvic function. For people with endometriosis it can treat secondary pelvic floor dysfunction that amplifies pain, helping patients regain comfort and daily activity.
How Does Pelvic Floor Dysfunction Make Endometriosis Pain Worse?
When pelvic floor muscles are tense, weak, or poorly coordinated they add mechanical stress and increase pelvic pain sensitivity. Dysfunction commonly causes ongoing pelvic pain, pain during intercourse, and urinary or bowel symptoms. Targeted physical therapy normalizes muscle tone, eases trigger points, and improves movement, often reducing symptoms.
What Techniques Are Used in Pelvic Floor Physical Therapy for Endometriosis?

Pelvic floor therapists use several strategies; common approaches include:
- Manual therapy : Hands-on release and stretching techniques to ease tight pelvic floor muscles and connective tissue.
- Biofeedback : Tools and cues that help you sense and retrain pelvic floor muscle activity for better control and relaxation.
- Education : Practical guidance about anatomy, pain science, posture, and self-care strategies to reduce flare-ups.
These are combined and individualized to promote relaxation, improve coordination, and gradually reduce pain.
Which Manual Therapy Modalities Can Relieve Endometriosis Symptoms?
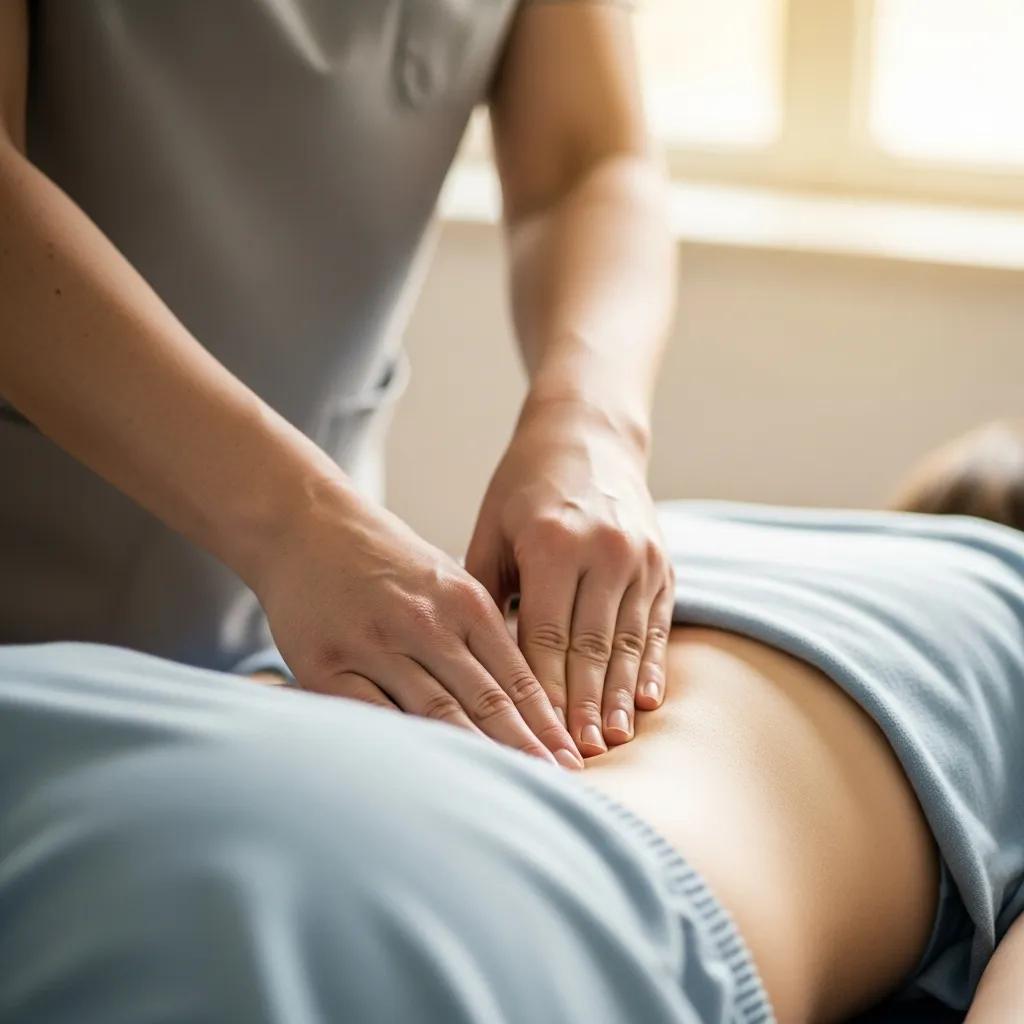
Manual therapy addresses soft tissue restrictions, scar mobility, and fascial tension that can contribute to pelvic pain; applied by trained clinicians it can reduce pain generators and improve function.
How Do Myofascial Release and Visceral Manipulation Help with Pelvic Pain?
Myofascial release targets tight fascia and muscles to restore mobility and reduce trigger points. Visceral manipulation addresses mobility of pelvic and abdominal organs and their connective tissue. Both aim to remove mechanical restrictions so movement causes less pain.
This approach aligns with research on myofascial dysfunction and central sensitization in persistent endometriosis-related pelvic pain.
Physical Therapy for Endometriosis: Addressing Myofascial Pain & Sensitization
Chronic pelvic pain in endometriosis often persists despite hormonal or surgical treatments because these approaches do not directly treat myofascial dysfunction or central sensitization. Myofascial trigger points and altered nervous system sensitivity can continue to generate pain. Interventions that target these mechanisms—such as physical therapy, dry needling, anesthetic injections, and botulinum toxin—are reviewed with attention to their proposed actions and clinical outcomes.
Relating chronic pelvic pain and endometriosis to signs of sensitization and myofascial pain and dysfunction, KJ Heyrana, 2017
What Does Scar Tissue Mobilization Do for Endometriosis Recovery?
Scar mobilization uses gentle techniques to soften adhesions and improve tissue glide after surgery or injury. When scars tether organs or limit mobility, mobilization can ease discomfort, restore range of motion, and support function during rehabilitation.
Which Physical Therapy Exercises Are Recommended for Endometriosis Pain Relief?
A thoughtful, individualized exercise plan restores pelvic mobility, strengthens support muscles, and improves movement without increasing pain.
Which Stretching and Strengthening Exercises Improve Pelvic Mobility?
Commonly recommended exercises include:
- Hip flexor stretches : Gentle stretches to reduce hip and pelvic tightness that can refer pain into the pelvis.
- Pelvic tilts : Controlled movements that improve core engagement and pelvic stability.
- Kegel exercises : When guided by a therapist, pelvic floor strengthening and relaxation exercises can restore balanced muscle function.
Therapists will tailor intensity and progressions to avoid flares and support steady recovery.
How Can Diaphragmatic Breathing and Relaxation Techniques Support Symptom Management?
Diaphragmatic breathing and relaxation reduce muscle tension and help regulate the nervous system. Slow, deep breathing and short relaxation routines can lower pelvic floor guarding, reduce stress-related pain amplification, and improve sleep and daily coping.
Consider consulting a pelvic health specialist at the Endometriosis Center of Excellence to discuss how physical therapy could fit into your care plan.
How Does Physical Therapy Fit into an Endometriosis Care Plan?
Physical therapy is a complementary element in comprehensive endometriosis care. It can be integrated before surgery, during conservative management, and after procedures to support symptom control and recovery.
What Is the Role of Pre-Operative Physical Therapy Before Excision Surgery?
Pre-operative therapy improves pelvic floor mobility and teaches strategies to reduce pain and aid recovery, often speeding postoperative recovery and lowering complications.
How Does Post-Operative Physical Therapy Support Recovery and Persistent Pain?
After excision or other pelvic surgery, targeted rehabilitation restores strength, mobility, and tissue flexibility, and addresses lingering pain, scar restrictions, and movement compensations to help patients return to activities.
The table summarizes common therapy types, techniques, and practical benefits in endometriosis care.
Physical therapy offers evidence-informed ways to reduce pain and improve function for people with endometriosis; understanding techniques helps you work with clinicians to build a plan that meets your goals.
Frequently Asked Questions
What are the potential side effects of physical therapy for endometriosis?
Most people tolerate therapy well; mild soreness or temporary increases in discomfort may follow hands-on work or new exercises and usually ease in a day or two. If pain worsens or persists, tell your therapist so they can adjust techniques or pacing.
How long does it typically take to see results from physical therapy for endometriosis?
Response varies: some patients improve after a few sessions, others need several weeks of consistent therapy. Progress depends on symptom severity, underlying issues, and adherence to the home program; regular re-evaluation refines the plan.
Can physical therapy be combined with other treatments for endometriosis?
Yes. Therapy complements medications, hormonal treatments, and surgery. By addressing pain generators and muscle function, it can improve symptom control and support recovery when coordinated with other treatments; discuss plans with your healthcare team.
Is pelvic floor physical therapy suitable for all women with endometriosis?
Pelvic floor therapy helps many people with endometriosis, especially those with pelvic pain or dysfunction, but it isn’t right for everyone. A skilled clinician will assess and recommend a tailored plan or alternatives.
What qualifications should a physical therapist have to treat endometriosis?
Look for a licensed physical therapist with specialized pelvic health training (e.g., DPT and postgraduate pelvic floor certification) and experience treating endometriosis.
How can I find a qualified physical therapist for endometriosis treatment?
Ask your physician for a referral or search professional directories such as the American Physical Therapy Association (APTA) for pelvic health specialists. Patient reviews and a brief consultation can help you assess fit.
Conclusion
Physical therapy is a practical, patient-centered part of endometriosis care that treats pelvic floor dysfunction and soft tissue restrictions contributing to pain. For a personalized plan, schedule an evaluation with a pelvic health therapist.

