Endometriosis lesions affect approximately one in ten reproductive-age women worldwide and often go unrecognized for years. Understanding endometriosis lesions begins with recognizing how patches of uterine-like tissue outside the uterus drive chronic inflammation, pain, and fertility challenges. In this comprehensive guide, you will learn what lesions are, how they develop, where they appear, and why they cause symptoms. We will explore the three main types of lesions—superficial peritoneal, ovarian endometriomas, and deep infiltrating—then detail the full spectrum of symptoms, diagnostic pathways from exam to laparoscopy, and the latest medical, surgical, and complementary treatments. You will also discover practical strategies for daily management, multidisciplinary support models, and emerging research in non-hormonal therapies and personalized medicine.
What Are Endometriosis Lesions and How Do They Affect the Body?

Endometriosis lesions are clusters of endometrial-like tissue that implant outside the uterine cavity, triggering chronic inflammation, scar formation, and organ distortion. These lesions respond to hormonal cycles, bleeding internally and causing adhesions that tether organs such as ovaries, bladder, and bowel. Persistent inflammatory signals sensitize nerve fibers and compromise organ function, leading to a multi-system disorder with pain and fatigue. Specialized centers apply advanced laparoscopic imaging and excision techniques to map and remove lesions with precision.
What Is an Endometriosis Lesion?
An endometriosis lesion is an ectopic deposit of endometrial glands and stroma located on peritoneal surfaces or within organs. It bleeds cyclically, provoking local irritation and fibroblast activation. Lesions vary in appearance—from clear, red-brown spots to dark “powder-burn” implants—and can fuse into plaques or nodules when chronic.
How Do Endometriosis Lesions Develop Outside the Uterus?
Retrograde menstruation is the predominant theory: menstrual debris flows through the fallopian tubes into the pelvic cavity, where viable endometrial cells adhere and proliferate. Alternative mechanisms include coelomic metaplasia of peritoneal cells, lymphatic or vascular dissemination, and stem cell implantation, all influenced by genetic predisposition and immune dysfunction.
What Are Common Locations for Endometriosis Lesions?
Common implantation sites include:
- Ovarian cortex, often forming endometriomas
- Peritoneal surfaces of the pelvis, bladder, and bowel
- Uterosacral ligaments, causing deep pelvic pain
- Rectovaginal septum, leading to dyspareunia
These strategic sites explain why adhesions distort anatomy and why women experience diverse symptom patterns.
How Do Endometriosis Lesions Cause Symptoms?
Lesions incite persistent inflammation and nerve sensitization, resulting in pelvic discomfort, worsening during menstruation. Adhesions tether organs, causing bowel and bladder pain. Cyclical bleeding within lesions provokes localized pressure and oxidative stress. Hormone-driven growth and regression amplify immune activation and fatigue.
What Are the Different Types of Endometriosis Lesions?
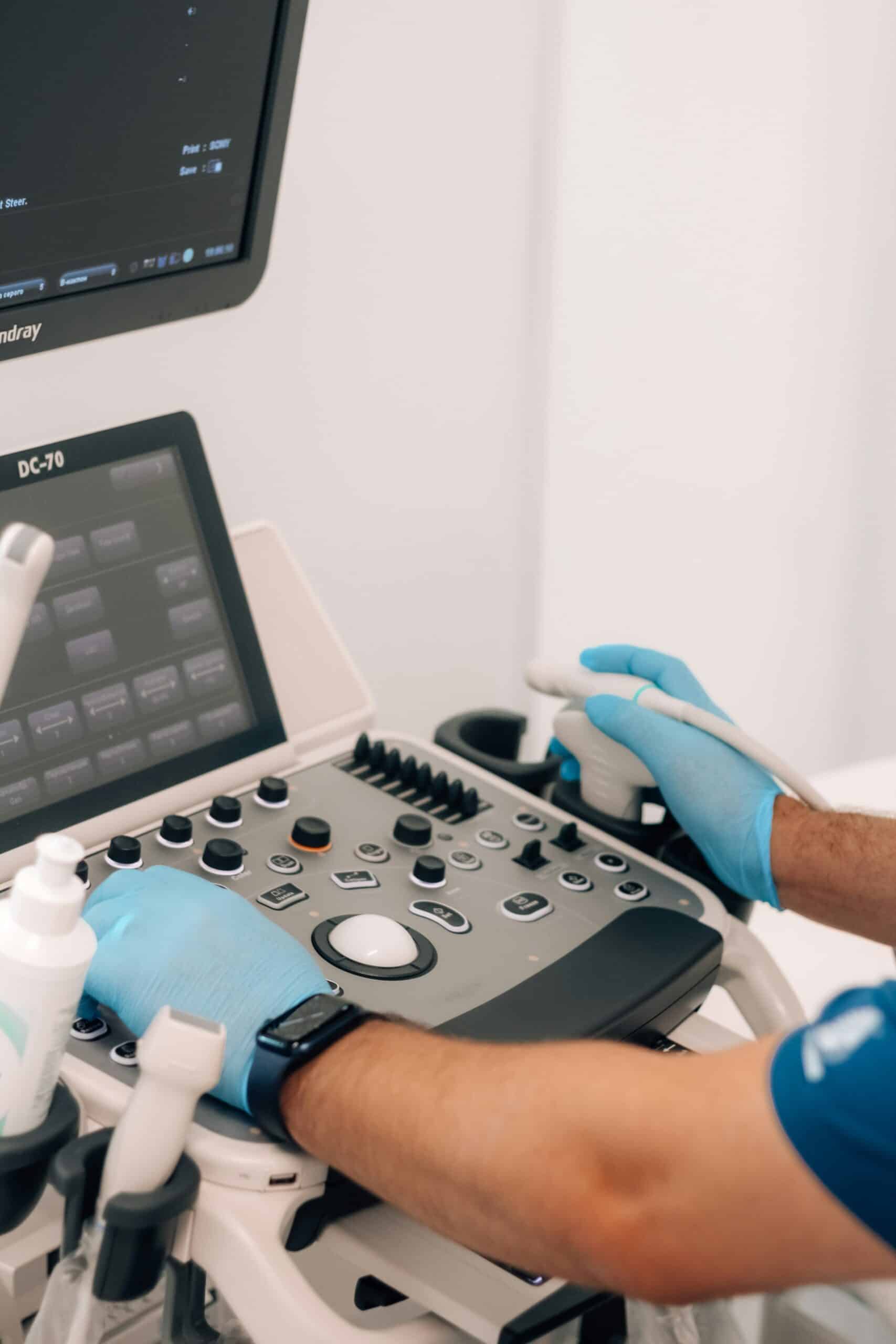
Lesion subtypes determine depth of invasion, symptom severity, and treatment strategies. Recognizing each type guides tailored management.
What Is Superficial Peritoneal Endometriosis?
Superficial peritoneal lesions are flat or slightly raised implants on pelvic peritoneum and ovarian surfaces. They remain within the peritoneal lining and cause mild to moderate inflammation. Pain often occurs during menstruation and intercourse, but fertility impact is variable.
What Are Ovarian Endometriomas (Chocolate Cysts)?
Ovarian endometriomas are cystic lesions filled with old blood, giving them a dark “chocolate” appearance. They invade the ovarian cortex, disrupt healthy follicles, and often present as painful masses. Infertility risk increases with cyst size and bilateral involvement.
What Is Deep Infiltrating Endometriosis and Why Is It Severe?
Deep infiltrating endometriosis (DIE) penetrates more than 5 mm beneath the peritoneal surface, affecting ligaments, bowel walls, bladder, and nerves. DIE induces significant scarring, organ dysfunction, and intense pain that often persists beyond menses. It requires specialized excision by experienced surgeons.
How Do Lesion Types Differ in Symptoms and Impact?
Different lesion types present distinct clinical profiles. The following table highlights key distinctions:
Each type requires a customized diagnostic and treatment plan that balances symptom control with fertility goals.
What Are the Common Symptoms of Endometriosis Lesions?
Symptoms vary widely but often include pelvic pain, menstrual cramps, painful intercourse, gastrointestinal distress, urinary discomfort, and profound fatigue. Recognizing the full symptom spectrum expedites diagnosis and improves outcomes.
How Does Chronic Pelvic Pain Manifest in Endometriosis?
Chronic pelvic pain is a persistent, non-cyclical ache or sharp discomfort in the lower abdomen and pelvis. It stems from inflammatory mediators, nerve sensitization, and adhesions that restrict organ mobility. Pain can intensify with movement, bowel activity, and sexual intercourse, significantly reducing daily function.
What Are the Signs of Dysmenorrhea and Dyspareunia?
Dysmenorrhea (painful periods) often presents as cramping radiating to the lower back and thighs, starting before or with menstruation onset. Dyspareunia (painful intercourse) arises when lesions in the uterosacral ligaments or rectovaginal septum are compressed during penetration, eliciting acute pain and emotional distress.
How Do Endometriosis Lesions Affect Gastrointestinal and Urinary Systems?
Lesions on the bowel cause painful bowel movements, bloating, constipation, or diarrhea, particularly during menses. Bladder implants lead to dysuria, frequent urination, and pelvic pressure. Gastrointestinal and urinary symptoms may mimic irritable bowel syndrome or interstitial cystitis, delaying correct diagnosis.
What Is the Impact of Endometriosis Lesions on Fatigue and Quality of Life?
Chronic inflammation and immune activation drain energy reserves, contributing to daily fatigue, mood disturbances, and sleep disruption. Quality of life suffers as pain, gastrointestinal symptoms, and fertility challenges intersect, underscoring the need for holistic care approaches.
How Are Endometriosis Lesions Diagnosed?
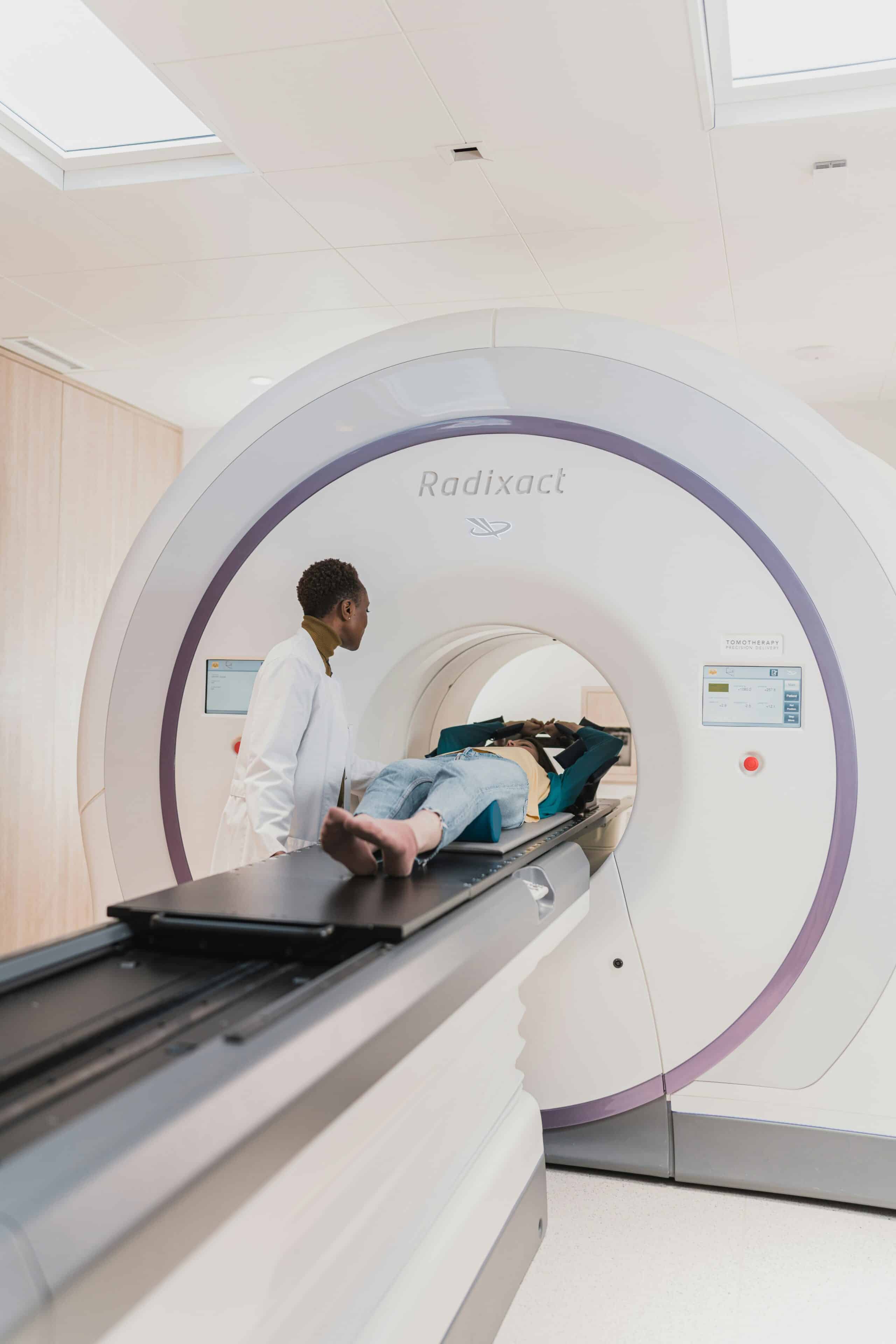
Accurate diagnosis blends clinical evaluation, imaging, and surgical confirmation. Early identification reduces the average 7–10-year diagnostic delay and guides effective treatment.
What Role Does Medical History and Physical Exam Play?
A detailed history uncovers pain patterns, menstrual cycle correlation, and symptom triggers. A pelvic exam may reveal fixed retroverted uterus, tender nodules along ligaments, or palpable ovarian masses, indicating potential lesions that warrant further investigation.
How Are Imaging Techniques Used to Detect Lesions?
Advanced ultrasound and MRI protocols improve detection of endometriomas and deep infiltrating disease. MRI offers superior soft-tissue contrast to map DIE in bowel, bladder, and ligaments, guiding surgical planning and multidisciplinary referrals.
Detailed imaging ensures precise lesion localization and tailored excision strategies.
Why Is Laparoscopy the Gold Standard for Diagnosis?
Laparoscopy allows direct visualization of lesions and adhesions, with the ability to perform targeted biopsy for histological confirmation. It remains the definitive diagnostic procedure and enables concurrent excision to relieve symptoms and improve fertility outcomes.
What Are Emerging Diagnostic Tools for Endometriosis Lesions?
Novel approaches include 99mTc-maraciclatide nuclear imaging to identify active lesions and molecular biomarkers in menstrual fluid for non-invasive screening. These innovations promise earlier detection and reduced reliance on surgical diagnosis.
What Are the Treatment Options for Endometriosis Lesions?
Treatment balances symptom relief, lesion removal, and preservation of reproductive potential. Options range from pharmacologic suppression to advanced excisional surgery and complementary therapies.
How Does Medical Management Help Control Symptoms?
Hormonal therapies—such as combined oral contraceptives, progestins, GnRH agonists, and antagonists—suppress ovarian estrogen production and reduce lesion activity. Non-steroidal anti-inflammatory drugs alleviate pain by inhibiting prostaglandin synthesis. Medical management can stabilize disease and defer surgery.
When Is Surgical Treatment Recommended?
Surgical excision is indicated for refractory pain, large endometriomas, deep infiltrating disease affecting bowel or bladder, and infertility after failed medical therapy. Minimally invasive laparoscopic excision performed by endometriosis specialists offers precise lesion removal while sparing healthy tissue.
What Are Complementary and Alternative Therapies?
Complementary approaches include pelvic floor physical therapy to release muscle tension, nutritional modifications emphasizing anti-inflammatory foods, acupuncture for pain modulation, and mindfulness-based stress reduction. These strategies support conventional treatment and improve quality of life.
How Do Fertility Treatments Integrate with Endometriosis Care?
Assisted reproductive technologies such as in vitro fertilization (IVF) can overcome lesion-related infertility when surgical correction and medical therapy are insufficient. Fertility preservation strategies, including egg or embryo freezing prior to extensive surgery, optimize reproductive outcomes.
How Can Patients Manage Life with Endometriosis Lesions?

Long-term management requires lifestyle adjustments, multidisciplinary support, and community resources to address physical and emotional challenges.
What Lifestyle Adjustments Help Alleviate Symptoms?
Regular low-impact exercise improves circulation and endorphin levels, while a diet rich in omega-3 fatty acids and antioxidants reduces inflammation. Heat therapy, adequate sleep, and stress management techniques further ease pain and fatigue.
How Does Multidisciplinary Care Improve Outcomes?
Collaborative teams of gynecologists, colorectal and urologic surgeons, pain specialists, physical therapists, and mental health providers deliver integrated care. Coordinating personalized treatment plans that address surgical, hormonal, nutritional, and psychological needs.
Where Can Patients Find Emotional and Community Support?
Support groups, both in person and online, connect patients with peers who understand the physical and emotional toll of endometriosis. Counseling services and patient advocacy organizations provide resources for coping strategies, educational materials, and referrals to expert care.
What Are Emerging Treatments and Research Developments for Endometriosis Lesions?

Research is focused on non-hormonal agents, advanced surgical modalities, and regenerative medicine to expand treatment choices and minimize side effects.
What Are the Latest Non-Hormonal Therapies Being Studied?
Dichloroacetate (DCA) shows promise in reducing lesion-associated pain by targeting metabolic pathways in endometrial cells. Immune-modulating biologics and anti-angiogenic agents are also under investigation to disrupt lesion growth without hormonal suppression.
How Are Advanced Surgical Techniques Improving Outcomes?
Robotic-assisted laparoscopy enhances precision in deep infiltrating excision, reducing complication rates and improving nerve preservation. High-definition 3D imaging and fluorescence-guided surgery facilitate complete lesion removal.
What Role Do Stem Cell and Personalized Medicine Therapies Play?
Autologous stem cell infusions and biomarker-driven treatment algorithms aim to regenerate healthy tissue, modulate immune response, and tailor interventions to each patient’s lesion profile and genetic background.
How Is Ongoing Research Changing Endometriosis Diagnosis and Treatment?
Large-scale clinical trials are evaluating non-invasive biomarkers for early screening, while genomic studies uncover gene variants associated with lesion aggressiveness. These insights will refine risk stratification and preventive strategies, moving toward a future of precision endometriosis care.
Endometriosis lesions represent a complex, chronic medical condition that demands comprehensive, expert-driven care. By understanding the nature of lesions, recognizing diverse symptoms, navigating diagnostic options, and accessing advanced treatments—both established and emerging—women can achieve significant relief and improved fertility outcomes. Coordinating personalized treatment plans that address surgical, hormonal, nutritional, and psychological needs.

