Endometriosis is a complex reproductive health condition that affects approximately 1 in 10 women of reproductive age. It occurs when tissue similar to the uterine lining grows outside the uterus, often on the ovaries, fallopian tubes, or pelvic lining. While it’s primarily known for causing chronic pelvic pain, its impact on fertility is equally significant—contributing to inflammation, anatomical distortion, and hormonal imbalances that can interfere with ovulation and embryo implantation.
For individuals trying to conceive, understanding the connection between endometriosis and infertility is critical. This blog explores how endometriosis affects reproductive health and outlines the most effective, evidence-based fertility options available today. From medical and surgical treatments to assisted reproductive technologies and supportive lifestyle strategies, we’ll provide a clear roadmap for navigating your fertility journey with confidence and clarity.
Key Takeaways
- Endometriosis is a chronic condition that can significantly affect fertility by causing inflammation, scar tissue, and anatomical distortions in the uterus and surrounding organs.
- A comprehensive treatment plan includes medical, surgical, and assisted reproductive technologies, each tailored to the patient’s individual symptoms and fertility goals.
- Lifestyle modifications, dietary changes, and supportive therapies play an essential role in managing endometriosis and improving fertility outcomes.
- Patients can benefit from working with experienced specialists who employ evidence-based protocols and cutting-edge technologies for precise diagnosis and treatment.
What Fertility Challenges Are Common With Endometriosis?
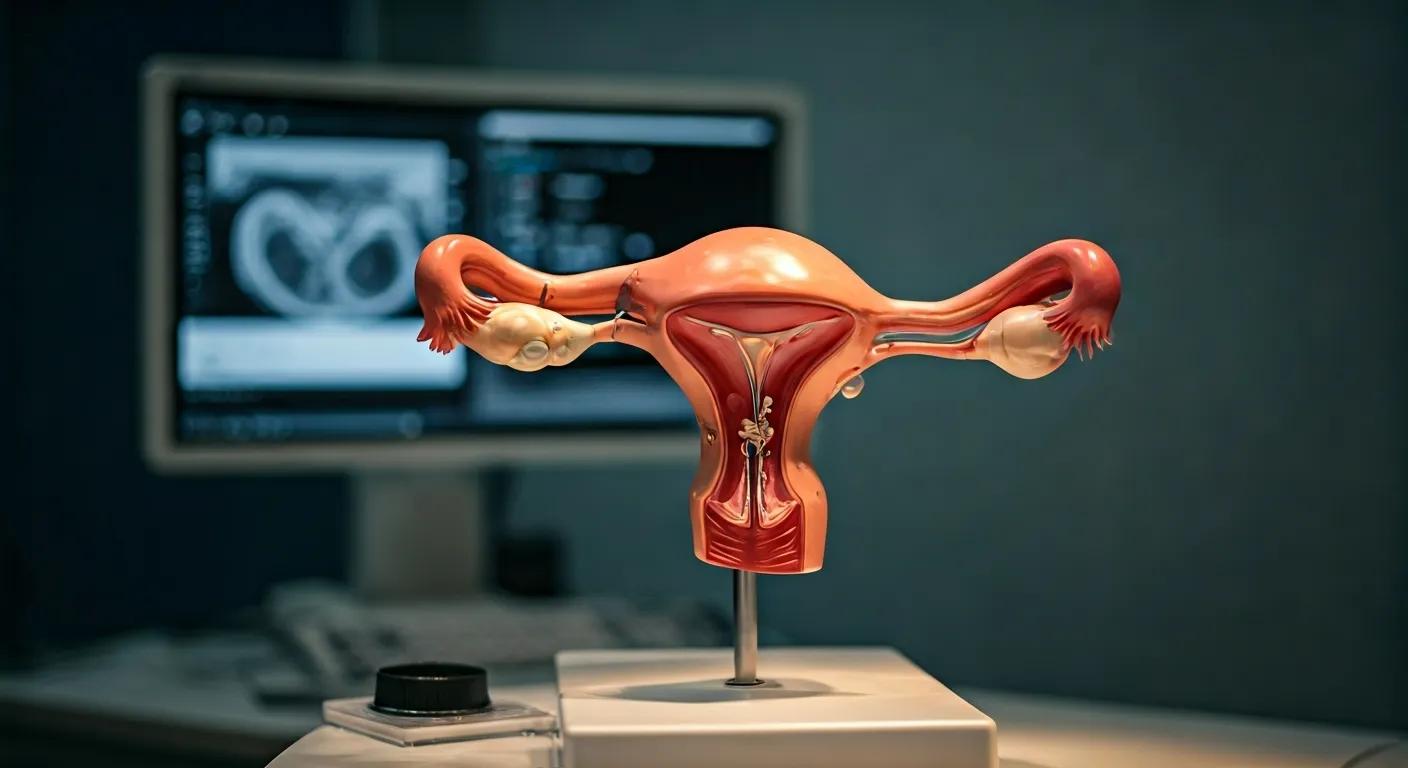
Endometriosis negatively impacts fertility by causing inflammation and adhesions that alter pelvic anatomy, reducing the mobility of the fallopian tubes and ovaries. This disruption makes it difficult for eggs and sperm to meet naturally. The condition can also compromise egg quality and the pelvic environment, leading to lower implantation rates and increased risk of miscarriage and ectopic pregnancy.
Additionally, endometriosis may coincide with other gynecological issues like adenomyosis or uterine fibroids, further distorting uterine shape and function. In some cases, the risk of pelvic inflammatory disease is higher, which can worsen scarring and inflammation. Because of these multiple factors, a multidisciplinary approach is needed to fully evaluate and treat the range of fertility issues associated with this condition.
How Does Endometriosis Cause Infertility?
Endometriosis causes infertility mainly through pelvic inflammation and structural changes. Inflammation hinders normal ovulatory function and disrupts gamete transport, while scar tissue can block or distort the fallopian tubes. The resulting hormonal imbalances also lead to a less receptive endometrial lining for embryo implantation, creating a challenging environment for conception.
What Is the Relationship Between Endometriosis and Ovarian Cysts or Fibroids?
Endometriosis is often linked with ovarian cysts, known as endometriomas, which form when endometrial tissue grows in the ovaries and damages surrounding healthy tissue. Furthermore, while uterine fibroids are separate benign tumors, their simultaneous presence with endometriosis can distort the uterus and further reduce fertility. Such overlapping conditions demand careful evaluation and, at times, a combined surgical approach.
Can Endometriosis Lead to Miscarriage or Ectopic Pregnancy?
The inflammatory environment created by endometriosis, along with anatomical distortions and adhesions, increases the risk of miscarriage and ectopic pregnancy. The endometrial lining may become less receptive to an implanting embryo, while adhesions can misdirect an embryo so that it implants outside the uterine cavity. This makes comprehensive treatment and close monitoring essential for affected women.
What Medical and Surgical Treatments Improve Fertility in Endometriosis Patients?
Medical and surgical treatments aim to reduce pain, control inflammation, and normalize pelvic anatomy to enhance fertility. Hormone therapy—using medications like Lupron (leuprolide acetate)—suppresses endometrial growth by inducing a temporary menopausal state and reducing inflammation, although it is a temporary solution for women planning pregnancy.
Laparoscopy is a commonly used, minimally invasive surgery to remove endometriotic lesions, release adhesions, and treat endometriomas while preserving ovarian tissue. In more severe cases, procedures such as endometrial ablation or hysterectomy may be considered for women who have completed childbearing. This surgical approach helps restore normal anatomy and reduces chronic inflammation, thereby improving fertility prospects.
Pain management is an essential adjunct to treatment. Non-steroidal anti-inflammatory drugs (NSAIDs) and other analgesics help control pain during the treatment process. A multidisciplinary approach that combines medical therapy, surgery, and supportive treatments gives patients the best chance for improved fertility outcomes.
How Does Hormone Therapy Help Manage Endometriosis Symptoms and Fertility?
Hormone therapy reduces estrogen levels using medications like GnRH agonists, progestins, or oral contraceptives. This minimization of hormonal fluctuations lowers inflammation and slows the growth of endometriotic tissue. Although effective in reducing pain and lesion size, these therapies are generally short-term and may be used alongside fertility treatments.
When Is Laparoscopic Surgery Recommended to Enhance Fertility?
Laparoscopic surgery is recommended for women with moderate to severe endometriosis who do not respond fully to hormone therapy or present significant anatomical distortions. The minimally invasive approach allows for the careful removal of lesions and adhesions, helping to preserve ovarian reserve and create a healthier environment for conception. Many specialists advocate for surgery before the initiation of assisted reproductive techniques like IVF.
What Are the Benefits and Risks of Surgical Treatments Like Endometrial Ablation or Hysterectomy?
For women who have finished childbearing, more definitive procedures such as endometrial ablation or hysterectomy may be considered. Endometrial ablation reduces menstrual bleeding and pain but is not suitable for those wishing to conceive. In contrast, a hysterectomy, which removes the uterus entirely, definitively treats endometriosis but eliminates the possibility of natural pregnancy. Both procedures carry the risks typical of major surgery, including infection and damage to nearby organs.
How Do Pain Management Strategies Support Fertility Treatment?
Effective pain control is vital for fertility treatment because chronic pain can disturb hormonal balance and increase stress. Regular use of NSAIDs, physical therapy, and complementary treatments such as acupuncture can reduce pain, improve sleep, and lower stress, creating a better overall environment for fertility treatments to succeed.
Assisted Reproductive Technologies (ART) for Endometriosis

For individuals with endometriosis-related infertility, assisted reproductive technologies (ART) offer effective pathways to conception when natural methods are less likely to succeed. Two of the most commonly used options are intrauterine insemination (IUI) and in vitro fertilization (IVF). These methods are designed to work around the structural and hormonal challenges caused by endometriosis.
How IUI Helps With Mild Endometriosis
Intrauterine insemination (IUI) involves placing specially prepared sperm directly into the uterus during ovulation. This technique shortens the journey sperm must travel and helps bypass minor obstacles such as limited tubal mobility or mild inflammation. IUI is typically recommended for patients with mild endometriosis and open fallopian tubes. It is less invasive and more affordable than IVF, though success rates may be lower in more severe cases.
IVF for Moderate to Severe Endometriosis
In vitro fertilization (IVF) is often the most effective fertility treatment for women with moderate to severe endometriosis. The process includes retrieving eggs from the ovaries, fertilizing them in a laboratory, and transferring healthy embryos into the uterus. IVF can overcome many of the anatomical and inflammatory barriers caused by advanced endometriosis, including scar tissue and distorted pelvic structures.
How Fertility Specialists Personalize ART Plans
Reproductive endocrinologists develop personalized treatment plans based on a detailed evaluation of hormone levels, ovarian reserve, and pelvic anatomy. Imaging studies, such as ultrasounds or MRIs, along with diagnostic history, help determine whether IUI, IVF, or a combination of both is the most appropriate course of action. This tailored approach improves the chances of successful conception while minimizing risks such as ovarian hyperstimulation or treatment failure.
What Lifestyle and Supportive Therapies Can Improve Fertility Outcomes With Endometriosis?

Lifestyle changes and supportive therapies can complement medical and surgical treatments for endometriosis, especially when fertility is a goal. While these approaches may not cure the condition, they can help reduce inflammation, regulate hormones, and support overall reproductive health—creating a more favorable environment for conception.
How Can Diet and Supplements Support Fertility?
Adopting an anti-inflammatory diet may help manage endometriosis symptoms and support hormone balance. Key strategies include:
- Increasing intake of fruits, vegetables, whole grains, and omega-3 fatty acids (such as from fish or flaxseed).
- Reducing processed foods, refined sugars, and trans fats that may contribute to inflammation.
- Using supplements like vitamin D, magnesium, curcumin, and antioxidants—which have been linked to reduced oxidative stress and improved hormonal function in some studies.
Always consult a healthcare provider before starting new supplements, especially during fertility treatment.
What Is the Role of Exercise and Stress Reduction?
Moderate physical activity helps improve blood flow, regulate insulin and hormone levels, and support healthy ovulation. At the same time, managing stress is essential for balancing cortisol and other hormones that influence fertility. Techniques such as:
- Mindfulness or meditation
- Gentle yoga
- Talk therapy or counseling
can help reduce stress and enhance emotional resilience during fertility treatment.
Can Acupuncture and Pelvic Floor Therapy Improve Fertility?
Certain complementary therapies may provide targeted benefits:
- Acupuncture is thought to improve pelvic circulation and reduce pain, and some evidence suggests it may improve endometrial receptivity for embryo implantation.
- Pelvic floor physical therapy addresses muscle tension and misalignment that can develop with chronic pelvic pain, potentially improving comfort and reproductive function.
These therapies are most effective when integrated into a comprehensive treatment plan under medical supervision.
Preparing for Fertility Treatment With Endometriosis: What to Expect

Fertility treatment for endometriosis begins with a complete evaluation to understand the severity of the condition and tailor the most effective care plan. This typically includes:
- Hormone level testing to assess reproductive hormone balance.
- Pelvic imaging (ultrasound or MRI) to identify cysts, scarring, or other anatomical issues.
- Ovarian reserve testing to evaluate egg quantity and quality.
- Diagnostic laparoscopy in some cases, to directly examine and possibly treat endometriotic lesions.
This detailed assessment helps fertility specialists recommend the right combination of medical, surgical, or assisted reproductive treatments.
What Should Patients Expect During the Process?
Fertility treatment with endometriosis can be a gradual journey. Some individuals may conceive after just a few cycles, while others may require longer-term care and multiple interventions. Expect the following during the process:
- In-depth discussions about treatment choices, timelines, and potential outcomes.
- A plan that may include hormone therapy, surgery, IUI, IVF, or a combination.
- Ongoing monitoring and adjustments based on treatment response.
- Emotional highs and lows, which are common when navigating fertility challenges.
How Do Lifestyle Changes Support Treatment Success?
Supportive habits like eating a balanced, anti-inflammatory diet, engaging in regular physical activity, and managing stress can improve how the body responds to treatment. These adjustments won’t replace medical care but may enhance hormonal balance and reduce inflammation, which are key factors in fertility.
Tracking menstrual cycles, symptoms, and treatment responses in a journal or app can also help providers refine the care plan over time.
Where Can Patients Find Expert Care and Resources for Endometriosis and Fertility?

Expert care for endometriosis involves connecting with specialists in reproductive endocrinology, gynecology, and minimally invasive surgery. Multidisciplinary care teams at reputable centers utilize advanced imaging, surgical techniques, and personalized treatment plans to address complex cases.
Patients should look for centers recognized for using evidence-based practices and often involved in clinical trials. Additionally, support organizations and advocacy groups offer valuable educational resources and community support, helping patients navigate both medical and emotional challenges.
Which Specialists and Clinics Are Best for Endometriosis-Related Fertility Care?
The top providers in this field are reproductive endocrinologists and gynecologic surgeons experienced in minimally invasive procedures such as laparoscopy. Dedicated centers of excellence for endometriosis and fertility preservation offer integrated treatment plans that combine surgical, medical, and supportive therapies.
What Organizations and Support Groups Offer Education and Advocacy?
Organizations like the Endometriosis Association and EndoFound, along with local support groups, provide educational materials, community forums, and seminars on treatment options and research updates. These resources empower patients with information and foster supportive networks.
How Can Patients Access Latest Research and Clinical Trials?
Patients can keep informed about emerging treatments by connecting with reputable medical centers and reviewing online platforms like ClinicalTrials.gov. Engaging with a fertility specialist involved in research ensures access to the most current treatment advancements and clinical trial opportunities.
Lifestyle and Supportive Therapies for Endometriosis and Fertility
The following table outlines supportive lifestyle therapies that enhance fertility outcomes:
Frequently Asked Questions
What is endometriosis, and how does it affect fertility?
Endometriosis is a condition where tissue similar to the uterine lining grows outside the uterus—often on the ovaries, fallopian tubes, or pelvic lining. This abnormal growth triggers inflammation, scarring, and anatomical changes that can interfere with ovulation, fertilization, and embryo implantation. Early diagnosis and targeted treatment are essential to improve fertility outcomes.
How do hormonal treatments like Lupron help manage endometriosis?
Hormonal therapies, such as GnRH agonists like Lupron, work by lowering estrogen levels to slow the growth of endometrial tissue. These treatments can reduce pain and inflammation, but they are typically temporary and are often used before or alongside fertility procedures—not as a long-term solution for those trying to conceive.
When is laparoscopic surgery recommended for fertility?
Laparoscopic surgery is recommended when medication alone does not manage symptoms or when pelvic adhesions, endometriomas, or significant structural issues are present. This minimally invasive procedure helps restore normal anatomy by removing lesions and scar tissue, often improving the chances of natural conception or success with assisted reproductive technologies.
Can lifestyle changes improve fertility in people with endometriosis?
Yes. Anti-inflammatory diets, regular exercise, stress reduction techniques, and supportive therapies like acupuncture can help regulate hormones and reduce inflammation. While not a standalone treatment, these lifestyle changes can enhance the overall effectiveness of medical and fertility interventions.
What assisted reproductive technologies are effective for endometriosis?
In vitro fertilization (IVF) is often the most effective option for moderate to severe endometriosis, especially when structural damage is present. Intrauterine insemination (IUI) may be suitable for milder cases. A fertility specialist will recommend the best approach based on the individual’s reproductive health and response to previous treatments.
How long does fertility treatment take for someone with endometriosis?
Fertility treatment timelines vary depending on age, disease severity, and how the body responds to therapy. Some patients may conceive within a few months, while others may need extended treatment over a year or more. Multiple cycles and ongoing plan adjustments are often part of the process.
Where can I find expert care for endometriosis-related fertility?
Look for clinics with expertise in reproductive endocrinology and minimally invasive gynecologic surgery. Multidisciplinary centers that offer advanced diagnostics, personalized care plans, and access to clinical trials typically provide the most comprehensive and effective treatment options.
Final Thoughts
Endometriosis significantly affects fertility through inflammation, anatomical changes, and hormonal imbalances. A tailored treatment plan involving hormonal therapy, minimally invasive surgery, and assisted reproductive technologies can markedly improve the chances of conception. Additionally, lifestyle modifications and supportive therapies are essential in creating an optimal environment for fertility. Working closely with specialized healthcare providers allows patients to overcome challenges and access the latest treatment options for improved reproductive outcomes.

